
Unmasking systemic injustice: racism, colonialism and the unequal burden of global health
Author:
Christian Djoko
Article Type:Article Number: 3
The world of global health, often lauded for its noble intentions and life-saving interventions, harbors an ugly side: a persistent undercurrent of racism, colonialism and power asymmetries that perpetuate inequalities and impede progress. This article looks at these structural problems in the global health ecosystem, exploring how they continue to shape health outcomes worldwide.
Context
The image of a white doctor in immaculate surgical scrubs, saving lives in a remote African village, has long dominated the global health narrative. While there is some truth to this image, it often masks the deeper complexities and injustices that continue to plague the global healthcare ecosystem. In reality, the struggle for global health equity is closely linked to issues of racism, colonialism, privilege and power asymmetries. To truly understand and address the challenges we face, we need to dismantle the façade and confront the shadow that lurks beneath.
The echoes and scars of colonialism
The legacy of colonialism casts a long shadow over global health. The exploitation and extraction of resources during the colonial era not only impoverished many regions, but also disrupted indigenous health systems and traditional knowledge. Colonial powers often imposed their own medical practices, disregarding local contexts and needs. The result was a system in which Western medicine became the gold standard, while traditional practices were marginalized and deemed “inferior” or retrograde.
The consequences of this situation are still being felt today. The lack of culturally appropriate health services, coupled with the high cost of Western medicines, prevents many communities from accessing adequate care. This is particularly true for marginalized groups, who are often discriminated against and excluded from “mainstream” healthcare systems.
Furthermore, medical research is sometimes carried out without the informed consent or involvement of the community. For example, the 1996 drug trials in Nigeria, carried out under the pretext of humanitarian action during a meningitis/measles epidemic, and the infamous Tuskegee experiments in the USA, where black men were unknowingly infected with syphilis, revealed a blatant disregard for the lives of marginalized communities. Such exploitative practices persist today in various forms, targeting vulnerable populations in developing countries. Pharmaceutical companies often prioritize profits over the lives and affordability of these populations.
The color of privilege and representation
Although international organizations are constantly striving for equity in global health, their structures can inadvertently or inherently perpetuate inequalities. Resource allocation, representation and decision-making power often reflect historical imbalances, hindering the development of fair, inclusive and effective global health practices that are adapted to the uniqueness of different cultural contexts.
Example: The under-representation of low- and middle-income countries in key decision-making bodies (Figure 1) contributes to the development of policies that may not adequately address the diverse health needs of the world’s population. A major report published in 2022 by the Global Health 50/50 revealed that the overwhelming majority of senior positions in international health organizations are held by individuals, in this case men from countries in the Global North (Figure 2).
Figure 1: The 15 most common nationalities among Board members of 146 organizations involved in global health.
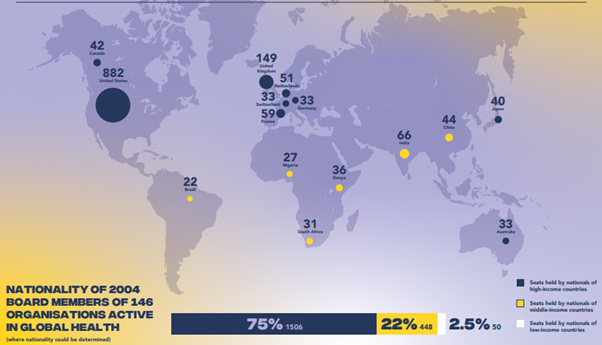
Source : Boards for All? Global Health 50/50 Report, 2022
Figure 2: Overview of 2014 Board seats in 146 organizations
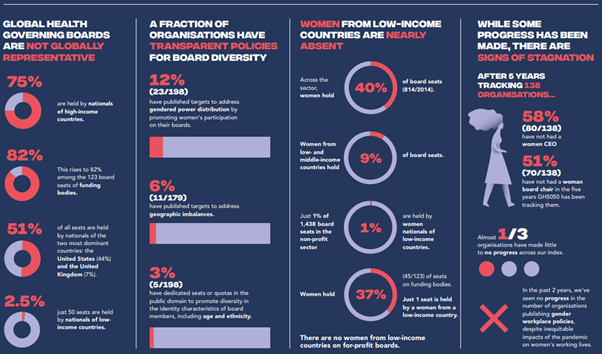
Source: Workplaces: Worse for Women, Global Health 50-50 Report, 2023
And the Global Fund?
Within this complex ecosystem, the Global Fund is regularly cited as an example to follow, despite the fact that there are still significant opportunities for improvement. According to the Global Health 50/50 Report 2022 (p. 39), the Global Fund stands out as a high-performing organization, scoring 6 or 7 out of 10 in the evaluation of 37 organizations. This recognition underlines the significant progress made by the Global Fund in implementing its missions.
An eloquent example of this performance is the composition of the Global Fund’s Board of Directors, made up of 20 voting members, with a balanced representation of implementers and donors. It should be noted that Africa, which is largely supported by the financial partnership, is currently lobbying for at least one additional seat on the Global Fund Board.
What’s more, the Board is appreciably diverse, both in terms of gender and North/South origin. However, particular attention needs to be paid to the Management Committee, where of the 13 members and the Inspector General, 3 are from countries in the Global South. This asymmetry underlines the importance of strengthening the representativeness of voices from less privileged regions, which concentrate the countries with the highest disease burden for each of the three diseases.
Beyond the governing bodies, the composition of the Global Fund’s operational teams also raises legitimate questions. Detailed data on the percentages of different nationalities among the Global Fund’s 1,300 employees are not available. An analysis of this national composition would provide a better understanding of the geographical distribution of expertise and help to ensure equitable representation (diversity and inclusion) of global perspectives in the decision-making processes of the Global Fund, whose headquarters are, as with almost all global organizations, located in the West (Figure 3).
Figure 3: Organizations in the sample are mainly headquartered in high-income countries
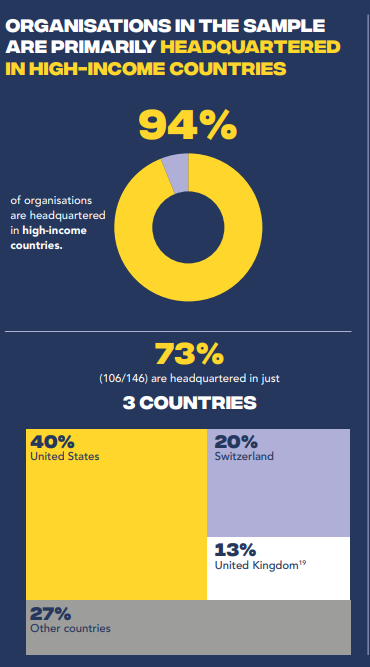
The lack of representation and diversity, and the global power dynamics that accompany it, are not limited to international organizations. It also manifests itself in epistemic inequalities and racial disparities in research funding between North and South, and especially within wealthy countries, creating imbalances between white and non-white researchers. Indeed, a study carried out in Great Britain in 2020 revealed that black and minority ethnic researchers face significant barriers to funding, publication and career advancement compared to their white counterparts (Figure 4). This perpetuates a cycle of exclusion and undermines the potential of diverse perspectives to contribute to better health outcomes.
Figure 4: Ethnic minority researchers face an unfair system compared to white researchers.
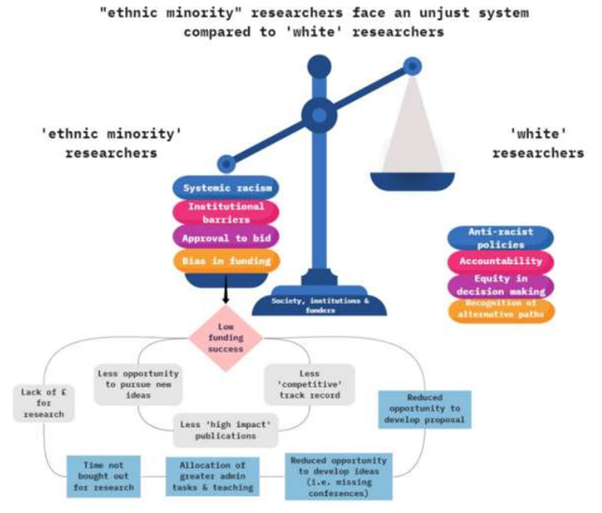
Source: Racism, equity and inclusion in research funding, 2021
The cost of power asymmetries
As we have just shown, the current global healthcare ecosystem is dominated by institutions and funding structures largely controlled by the West. Power imbalances and privileges in this global health hierarchy create a “donor-recipient” dynamic, in which decisions on research priorities, interventions and resource allocation are often made without the input of the communities most affected by global health problems. High-income countries often exert a disproportionate influence, reinforcing a global health landscape where the powerful dictate the global health agenda. This can lead to the neglect of diseases that disproportionately affect low- and middle-income countries, such as neglected tropical diseases (NTDs). Comprising a diverse set of 20 diseases, these conditions receive a minimal portion of global health funding, despite their impact on more than a billion people worldwide, including 400 million in Africa.
According to a study carried out in 2022 as part of WHO Africa’s expanded special project to eliminate neglected tropical diseases, nearly 99 million people in 26 African countries are at risk this year of being denied access to treatment for conditions such as lymphatic filariasis, onchocerciasis, geohelminthiasis and schistosomiasis. More broadly, neglected tropical diseases impose a heavy socio-economic and educational burden on the patients and families affected. According to a WHO study aimed at justifying continued investment in the eradication of these diseases, the loss of household income linked to healthcare expenditure and jobs lost as a result of these conditions is estimated at a minimum of 33 billion US dollars per year. By way of illustration, human African trypanosomiasis in the Democratic Republic of Congo generates costs representing over 40% of the annual income of affected households in a typical rural community. Similarly, up to 75% of households affected by visceral leishmaniasis in Bangladesh, India, Nepal and Sudan face financial difficulties in accessing diagnosis and treatment, even when tests and medicines are theoretically free.
This imbalance in the priorities of global health initiatives is often exacerbated by a glaring shortfall in domestic health funding by Southern states (the culpable responsibility of local leaders), as well as by the profit motives of pharmaceutical companies. The latter give priority to developing drugs for diseases prevalent in rich countries. Example: Unequal access to essential medicines and vaccines. The COVID-19 pandemic has once again vividly highlighted this problem. Initial access to vaccines was privileged for wealthy countries, securing their vaccine supply, while many African countries struggled in vain to obtain sufficient doses, resulting in millions of avoidable deaths.
Racism, linked to colonialism, also exacerbates these deadly inequalities, and has done so for a long time. Prejudice based on race, ethnicity and nationality influences access to healthcare, treatment and research priorities. Black and brown communities are often discriminated against in healthcare facilities, leading to misdiagnosis, delayed treatment and poorer health outcomes. As Winnie Byanyima, Executive Director of UNAIDS, points out in a recent article:
|
It is often said that illnesses do not discriminate. When we look at the effect of health crises, however, it is clear that African people, people of African descent and other racialised groups are hit harder, because of the systemic nature of racism. Racism is deadly not only when people can no longer breathe because of police violence. Racism is deadly when people take their last breath because of policy violence, including global and national policies that result in people being unable to get the medicines or care that could save their lives. |
All of the above underscores the urgent need to dismantle systemic racism in the in the global healthcare ecosystem and in many national healthcare systems.
The status quo is not an option
Tackling the deep-seated problems of racism, colonialism and power asymmetries in global health requires a multi-pronged approach. First, we must acknowledge the historical and current injustices that have shaped the current landscape. This means dismantling the white savior narrative and acknowledging the expertise and knowledge of the communities most affected by health disparities.
Second, we need to invest in building a more diverse and equitable global health workforce. This includes supporting researchers and health professionals from low- and middle-income countries, promoting culturally competent care and ensuring equal access to opportunities and resources.
Thirdly, the global health agenda needs to be democratized, with greater representation and participation of the communities most affected by health problems. This means changing power dynamics. It is essential that the voices and expertise of those most affected by global health issues are heard. Community-led research and program development can ensure that interventions are culturally relevant and effective.
Fourth, equity in representation must be established. Increasing diversity in leadership positions and research teams within global health organizations is essential to ensure inclusive and effective solutions.
Conclusion
The fight for equity in global health isn’t just about providing medical care; it’s about dismantling the structures of racial and colonial injustice that perpetuate health disparities. By acknowledging the shadow, confronting its roots and working towards a more equitable future, we can build a truly fairer and more inclusive global health ecosystem that leaves no one behind.
