
Navigating the transition: Sustainable strategies for health care funding in the Eastern Mediterranean Region
Author:
Samuel Muniu and Amida Kariburyo
Article Type:Article Number: 4
The Eastern Mediterranean Region Constituency of the Global Fund held its annual meeting in Tunisia, attracting government officials, healthcare professionals, and international organization representatives. This article summarizes the discussions, which highlighted the need to enhance healthcare access and transition from Global Fund support to domestic resources. This shift is vital for achieving self-reliance and sustainability, particularly in combating HIV, Tuberculosis, and malaria.
The Eastern Mediterranean Region Constituency (EMRC) of the Global Fund Board, consisting of 15 countries, held its annual meeting in Tunisia from February 27th to 29th, 2024. The event drew government officials, healthcare professionals, and representatives from international organizations. Discussions focused on improving healthcare access and constituency engagement in the region, including emphasis on transitioning from Global Fund support to domestic resources. This transition is vital for achieving self-reliance and sustainability in healthcare systems, particularly in the fight against HIV, Tuberculosis (TB), and malaria. In this article, we explore the insights garnered from the EMRC meeting, with a specific focus on sustainability and the transition from Global Fund support to domestic resources.
Background
The World Health Organization (WHO) estimates that in the Eastern Mediterranean Region (EMR) in 2022, approximately 490,000 people had HIV, but only 38% knew their status, and 27% were receiving treatment. About 130,000 individuals received antiretroviral therapy. HIV-related deaths surged by 72% to 20,000 between 2010 and 2022. In 2020, the TB rate was 112 per 100,000 population, contributing nearly 8% to global cases, with Pakistan (70%) and Afghanistan (9%) having the highest proportions. In the same year, 80,000 TB patients without HIV died in the region. Among the Eastern Mediterranean Region’s seven malaria-endemic countries in 2022, they represented 3% of global malaria cases. Sudan had the highest malaria burden at 41%, followed by Pakistan, Somalia, Yemen, Afghanistan, and Djibouti.
Global Fund in the Eastern Mediterranean Region
The Eastern Mediterranean Region Constituency of the Global Fund comprises 15 countries in the Middle East and North Africa (Figure 1).
Figure 1: Global Fund Eastern Mediterranean Region Constituency

Source: EMRC
Nine countries in the EMRC are expected to transition from Global Fund financing by 2028: Djibouti for malaria, Egypt for TB, Iran for HIV, Iraq for TB, Jordan for TB, Libya for TB, Namibia for HIV, TB, and malaria, Pakistan for malaria, and Palestine for HIV and TB.
Mohamed Chakroun, head of the Infectious Diseases Department at Fattouma Bourguiba University Hospital in Monastir and chair of Tunisia’s Country Coordinating Mechanism (CCM), serves as the Global Fund Board member for the region. Mohsen Asadi-Lari, a professor of epidemiology at Iran University of Medical Sciences in Tehran and a CCM member in Iran, serves as the alternate member for the region.
Between the 2023-2025 and 2020-2022 cycles, Global Fund funding for the region went up (Figure 2).
Figure 2: Global Fund funding to EMR
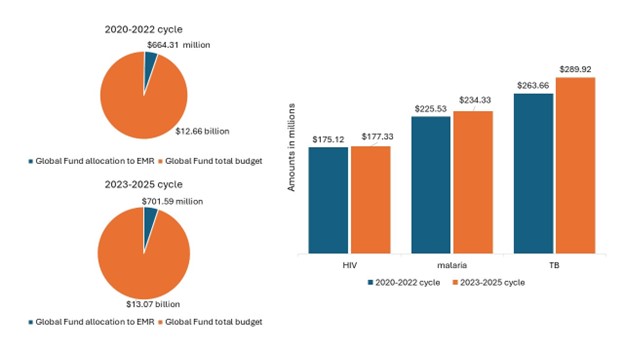
Source: Global Fund Data Explorer
EMRC Meeting Highlights
The concept of sustainable transition in healthcare, as outlined by the International Health Partnership for Universal Health Coverage (UHC), is the ability of a health system to maintain or improve coverage of priority interventions like HIV, TB, and malaria while progressing towards universal health coverage. This transition relies on two key pillars: financial sustainability and enhanced efficiency.
Financial sustainability involves governments increasing domestic allocations for essential health interventions, aligning health spending with economic growth. This is crucial for reducing dependence on external funding sources, ensuring long-term stability in healthcare provision. Enhanced efficiency, the second pillar, entails integrating HIV, TB, and malaria services with broader healthcare initiatives. Utilizing innovative technologies and implementation methods optimizes resource utilization and service delivery, contributing significantly to sustainable healthcare systems.
Indeed, Ghada Muhjazi, Technical Officer at the WHO Regional Office for the Eastern Mediterranean, emphasized, “Efforts to improve efficiency can be done through integration or better alignment of HIV, TB, malaria services with other health services, or by introducing innovative cost-effective technologies and implementation methods.”
The Global Fund Sustainability, Transition and Cofinancing (STC) policy underscores the importance of embedding sustainability principles into all strategic documents, including National Strategic Plans and funding requests. By prioritizing sustainability, countries mitigate the risk of performance decline or collapse when transitioning from Global Fund support. Whether transitioning gradually or abruptly, a steadfast commitment to sustainability principles ensures the continued success of healthcare programs.
Advancing financial sustainability
The meeting underscored financial sustainability as a cornerstone of the transition process. A literature review conducted in the Eastern Mediterranean region has shed light on the opportunities and challenges in strengthening sustainability within healthcare, particularly concerning HIV, TB, and malaria programs. One significant finding highlighted the relatively low dependency on external financing for overall health spending in the region, with only a few countries relying on the Global Fund (Figure 3). This suggests the potential for increased domestic allocations.
Figure 3: EMRC dependence on external financing for overall health, as a percentage of total, 2019
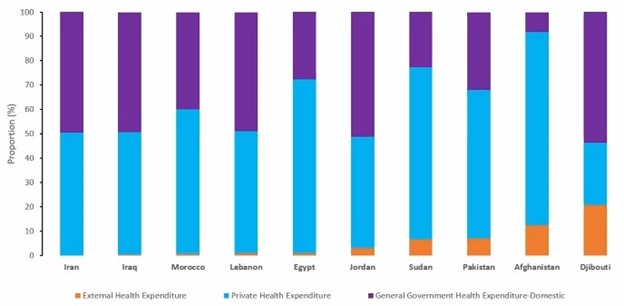
Source: EMRC meeting presentation
However, the review also revealed a stark contrast in funding for HIV, TB, and malaria programs, with a significant reliance on Global Fund support observed (Figure 4). For instance, the analysis found that the majority of countries in the region heavily depend on Global Fund support for malaria and TB, with over 75% of funding sourced externally. Similarly, several countries rely on the Global Fund for over 50% of their HIV program funding. This imbalance underscores the urgent need to diversify funding sources and enhance domestic allocation for these critical diseases.
Figure 4: Dependence on Global Fund financing for HIV, TB, and malaria in EMRC
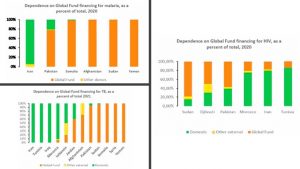
Source: EMRC meeting presentation
This dependence on external funding for specific diseases underscores the need for diversification of funding sources and increased domestic allocations to ensure the sustainability of these critical health interventions. The commitment to achieving UHC by the EMRC presents a promising opportunity (Figure 5). If countries uphold this commitment, it signifies a shift towards sustaining and expanding coverage of priority interventions, including HIV, TB, and malaria. This entails not only increasing domestic allocations but also improving efficiency in healthcare delivery.
Figure 5 : A commitment to UHC by EMRC countries
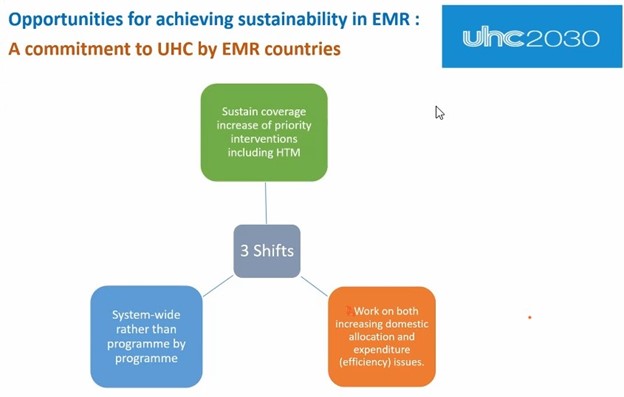
Source: EMRC meeting presentation
COVID-19 response lessons: recognizing the need for increased healthcare funding
The meeting served as a platform to discuss the lessons learned from the COVID-19 pandemic. While it has undoubtedly caused devastation and impacted societies worldwide, the response to COVID-19 has also presented invaluable lessons and opportunities for enhancing healthcare systems despite the chaos and challenges. One crucial lesson learned from the pandemic is the heightened awareness among policymakers regarding the importance of investing in healthcare. The pandemic has underscored the critical role of a robust healthcare system in safeguarding public health and ensuring economic stability. As a result, there is now a greater recognition of the need for increased allocation of domestic resources towards healthcare, including essential services such as those for HIV, TB, and malaria.
These innovative strategies, born out of necessity during the pandemic, have demonstrated their effectiveness and cost-efficiency. As we move beyond the acute phase of the COVID-19 crisis (Figure 6), it is imperative to capitalize on these lessons and integrate these practices into routine healthcare delivery. By doing so, we can enhance the resilience of our healthcare systems and better prepare for future health emergencies.
Figure 6: COVID-19 management
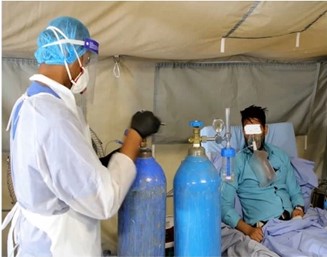
Source: EMRC meeting presentation
Furthermore, the pandemic has highlighted the importance of prudent financial management and investment in healthcare infrastructure. Redirecting funds towards building resilient healthcare systems can help mitigate the impact of future crises and ensure that communities are better equipped to respond to emerging health threats.
Challenges to achieving healthcare sustainability in the EMRC
From the meeting, it emerged that political instability and regional disasters have posed significant obstacles to healthcare sustainability, leading to a heavy reliance on external donor support. Yemen’s situation exemplifies this, as before the 2014 crisis, the country allocated approximately $1 million domestically to its malaria program. However, funding was entirely halted post-crisis, leaving Yemen dependent solely on organizations like the Global Fund. Similarly, Iraq faced setbacks in transitioning due to crisis situations, necessitating a return to reliance on external aid, despite some domestic resources still being allocated, falling short of meeting healthcare needs adequately.
Another pressing challenge highlighted is the inadequate access to healthcare for migrant populations and internally displaced persons (IDPs). Many countries lack explicit provisions in their health policies to effectively address the healthcare needs of these vulnerable groups. Consequently, they encounter barriers to accessing essential healthcare services, exacerbating health disparities within the region.
Additionally, despite the region’s comparatively lower revenues, concentrated HIV epidemics persist. Experts have noted a worrying increase in new HIV infections, accompanied by social and cultural barriers hindering access to care for key and vulnerable populations. This underscores the urgent need for targeted interventions and policy reforms to address these disparities and ensure equitable healthcare access for all segments of society.
Navigating healthcare sustainability: Key considerations
Within healthcare governance, critical factors necessitate immediate attention to fortify sustainability and navigate the transition toward greater self-reliance. Discussions during the meeting delved into these key areas, highlighting the need for focused attention and strategic initiatives.
Establishing a dedicated sustainability unit
To kickstart the journey towards sustainability, it’s imperative to institute a dedicated sustainability unit vested with the responsibility and authority to spearhead and oversee the transition process. This unit will play a pivotal role in planning, coordinating, and driving initiatives aimed at achieving sustainability goals. By centralizing accountability and leadership within this unit, the process gains coherence and direction, ensuring effective planning and execution.
Enhancing the role of existing institutions
While advocating for the establishment of a sustainability unit, it’s also crucial to optimize the existing governance structures. Rather than abolishing entities like the CCM, there’s a need to augment their role and embed them within national institutions. This strategic integration fosters greater accountability and allows for leveraging the expertise and insights gained through these mechanisms. Furthermore, expanding representation within the CCM ensures diverse perspectives and promotes inclusive decision-making.
Engaging diverse stakeholders
Sustainability efforts necessitate collaboration across various sectors and stakeholders. Involving entities such as the Ministry of Finance, legislative bodies, private sector, and civil society is paramount. The private sector, in particular, can play a pivotal role not only in advocating for resource allocation but also in driving innovation and efficiency within healthcare systems. However, such engagement must be accompanied by robust frameworks to manage conflicts of interest and ensure alignment with broader public health objectives.
Financial planning and analysis
A comprehensive analysis of financing data is indispensable for informed decision-making and strategic planning. This entails tracking healthcare spending, assessing funding gaps, and identifying opportunities for enhancing domestic resource allocation. Tools such as the Funding Landscape Tool proposed by global health organizations can provide valuable insights into financing dynamics and guide resource allocation strategies. Additionally, gradual transition towards domestic financing models prepares healthcare systems for long-term sustainability, reducing dependency on external funding sources.
Strengthening service delivery
Efforts to enhance service delivery must prioritize the integration of essential healthcare services, including HIV, TB, and malaria, within primary healthcare systems. This integration ensures comprehensive and holistic care delivery while optimizing resource utilization. Engaging private sector providers can further augment service delivery capacity, provided it is accompanied by stringent quality control measures and regulatory oversight. Moreover, addressing workforce challenges and aligning salary scales are essential for retaining skilled personnel and ensuring continuity of care.
Optimizing health products and supply chains
Efficient procurement and supply chain management are essential pillars of sustainable healthcare systems. Progressive transition towards domestic procurement, integration of supply chains, and capacity-building initiatives are imperative. Streamlining regulatory processes and exploring alternative procurement mechanisms can expedite access to essential health products while mitigating bureaucratic hurdles. Additionally, leveraging partnerships with international agencies can facilitate access to vital supplies, particularly in regions facing sanctions or supply chain constraints.
Empowering vulnerable populations
Effective healthcare governance entails prioritizing the needs of vulnerable populations and fostering inclusivity within healthcare systems. This necessitates addressing attitudinal barriers among healthcare workers and law enforcement personnel, as well as optimizing the role of civil society organizations (CSOs). Social contracting with CSOs can complement governmental efforts in reaching marginalized communities, ensuring continuity of care beyond the scope of donor funding. Moreover, investing in the sustainability of CSOs is essential for long-term resilience and community engagement.
Conclusion
Navigating towards healthcare sustainability requires proactive measures across governance, financing, service delivery, and stakeholder engagement. While significant strides have been made in combating diseases like HIV, TB, and malaria, sustaining these achievements demands concerted efforts and strategic foresight. By fostering collaboration, optimizing resource allocation, and prioritizing inclusivity, healthcare systems can navigate the transition towards self-reliance with resilience and efficacy. Ultimately, achieving sustainability heralds a triumph of national self-reliance and autonomy, reflecting a commitment to equitable healthcare access and enduring health outcomes.
