The conclusions of the Future of Global Health Initiatives process (Lusaka Agenda): What can we expect?
Author:
Ida Hakizinka et Christian Djoko
Article Type:Article Number: 2
December 12, 2023 marked the launch of the Lusaka Agenda. It proposes an action plan for a shared, long-term vision of nationally-funded healthcare systems, as well as Universal Health Coverage (UHC) that leaves no one behind. To achieve these objectives, the Agenda proposes five major changes. This article presents a critical assessment of these changes. Will the ideal pass the reality test?
What is the Lusaka Agenda?
The global health financing landscape is dense and often complex to grasp (Figure 1). A multitude of players are involved, from national governments to international organizations, philanthropic bodies and private companies. Each of these players has its own objectives, priorities and funding mechanisms, creating a tangle that is sometimes difficult to untangle for those seeking to understand the overall workings of the healthcare system. What’s more, funding policies and strategies are constantly evolving in response to demographic, economic and political changes, adding another layer of complexity to this already dense environment.
Figure 1: Flows of global health financing in 2021
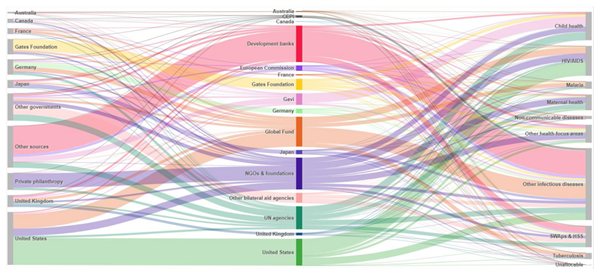
Source: Reimagining the Future of Global Health Initiatives
Consequently, navigating this landscape requires in-depth understanding and careful analysis to identify the gaps, opportunities and challenges to ensuring adequate and equitable financing for health worldwide. This is where the Lusaka Agenda comes in. This international initiative officially launched on December 12, 2023, celebrated as Universal Health Coverage Day, aims to propel the Global Health Initiatives (GHIs) and the wider health ecosystem towards a vision of nationally financed health systems and universal health coverage (UHC). It is the result of a multi-stakeholder dialogue, marked by the Wilton Dialogue as a pivotal moment (see the list of participating GHIs, implementing partner countries, donors, CSOs here), in the Future of Global Health Initiatives (FGHI) process.
Discussions focused primarily on national GHIs such as Gavi, the Global Fund to Fight AIDS, Tuberculosis and Malaria, and the Global Financing Facility (GFF -hosted at the World Bank), but also included other key players such as Coalition for Epidemic Preparedness Innoations (CEPI), Unitaid and Foundation for Innovative New Diagnostics (FIND). Representatives from donors, governments, global health organizations, civil society and research participated to ensure an aligned and coherent approach. The Lusaka Agenda represents a consensus on a number of changes for the long-term evolution of GHIs (Figure 2).
Figure 2: Process leading up to the Lusaka Agenda and follow-up
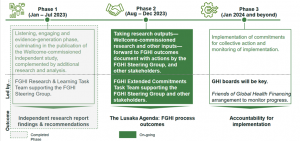
Source: Global Alignment Agenda Country Impact, Global Financing Facility 2023
Recommended changes
The Lusaka Agenda recommends five main changes:
- Strengthen the contribution to primary health care (PHC) by effectively strengthening health systems: GHIs are expected to make a greater contribution to PHC by effectively strengthening health systems. The aim is to improve access to essential services, promote preventive measures and guarantee local care.
- To act as a catalyst for national and sustainable financing of health services and public health functions: this can reinforce sustainability and reduce dependence on external sources of funding.
- Strengthen joint approaches to achieving equity of health outcomes: ensuring that health services are distributed equitably and reach marginalized populations.
- Ensure strategic and operational coherence: streamlining efforts and resources to achieve common health objectives.
- Coordinate approaches to products, research and development (R&D), and regional manufacturing to address market and policy failures related to global health: encouraging innovation and progress in healthcare delivery.
This perspective implies a significant transition in the way health interventions are designed and implemented:
- Implementing countries are taking an increasingly proactive role in identifying priorities for equitable, essential and cost-effective interventions. This is based on their own capacity and financial resources.
- Donors delegate more responsibility for implementation to recipient countries, demonstrating greater risk tolerance and accepting more comprehensive public health outcomes, with a focus on primary healthcare.
- GHIs support countries in this transition by focusing on sustainability, adopting a more flexible operational approach to respond to evolving national capacities, and ensuring that their investments complement domestic and other external funding sources.
For the Agenda’s authors, this approach aims to strengthen national ownership of health programs, increase the effectiveness of interventions and promote more efficient use of available resources, while fostering greater accountability among national and international players involved in the health sector.
The timetable for implementing the Agenda’s recommendations
These changes reflect the evolving global health context, marked by shifting funding priorities, potential reductions in donor funding and the need for countries to work differently to address a range of health-related issues, such as epidemics, climate change, economic constraints and evolving epidemiology. By focusing on these changes and setting short-term priorities to catalyze action in this direction, the Lusaka Agenda provides the roadmap for coordinated action to support these changes and move towards a vision of nationally-financed health systems and a UHC.
The timetable for implementing the recommendations includes GHI’s involvement in pioneer countries to highlight the different levels of maturity of systems. The timetable sets out a framework for joint working and supervision, simplified grant processes and transparent financial flows to create an effective health financing system that makes an impact, particularly in times of limited resources. Finally, the Agenda stresses the importance of united and collective efforts by all stakeholder groups to achieve these changes, underpinned by mutual accountability. In order to operationalize these changes and actions in the short term, the Lusaka Agenda issues a call to action (Figure 3) to all stakeholders involved in national leadership.
Figure 3 : Lusaka Agenda : Call to action
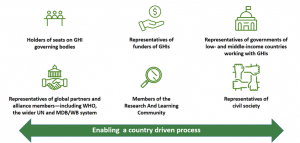
Source: Global Alignment Agenda Country Impact, Global Financing Facility 2023
The designers and authors of this Agenda put forward the idea that their aim is not to consolidate or modify existing mandates, but rather to promote specific long-term changes that each GHIs should autonomously foster in order to better support countries. At this stage, however, there is no evidence to support this hypothesis. There are even grounds for reasonable doubt.
Issues and challenges
While the Agenda represents an indispensable step towards a more equitable and sustainable future for global health, closer examination reveals important issues and challenges that require our attention.
Changing power dynamics: A laudable goal, but how achievable?
The heart of the Lusaka Agenda lies in its call for a paradigm shift. It emphasizes a shift away from vertical, donor-driven programs to a GHIs’ landscape characterized by country ownership, shared leadership and context-specific approaches. This is a welcome change, which resonates deeply with concerns about the paternalistic approaches of the past, which often relegated recipient countries to passive roles. But isn’t the realization of this aspiration wishful thinking and overly naive? Are traditional donors really willing to relinquish control? Will recipient countries have the financial and technical capacity to take the reins?
Firstly, dismantling entrenched power structures within the global health financing architecture is no mean feat. Some established donors wield considerable influence, and their willingness to relinquish control remains to be demonstrated. Concrete incentives need to be created to encourage a shift towards flexible, long-term financing models that prioritize national health plans over pre-established agendas.
Secondly, strengthening country ownership depends on the strength of health systems in recipient countries. Many developing countries lack the infrastructure, human resources (indeed, there is no mention of the term “human resources” in the Agenda) and financial capacity to effectively lead and manage their health priorities. It’s up to the GHIs to provide targeted capacity-building support, ensuring that recipient countries have the technical expertise and governance structures needed to lead their own health destinies.
Financing the future: aligning interests? Yes, but will the money follow the rhetoric?
At the heart of the Agenda is the quest for a more coherent, equitable and efficient global health financing architecture. It envisages the establishment of a system in which funding flows are harmonized according to national priorities, as well as greater collaboration between the main health institutions. This vision is to be welcomed, and its fulfillment is more crucial than ever. This is particularly necessary for healthcare providers in African countries, who often find themselves faced with a multitude of different application processes, evaluations and accountability systems between these organizations or GHIs.
However, some skepticism remains. This is not the first attempt to set up such alignment processes, and many have failed as this overview shows (Figure 4).
Figure 4: Timeline of GHI establishment and coordination efforts since 2000
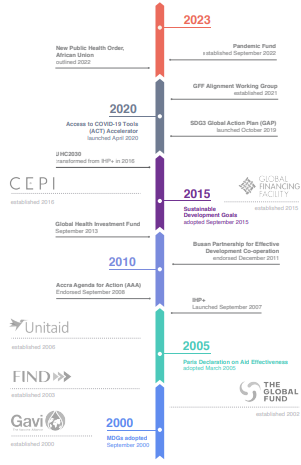
Source : Reimagining the Future of Global Health Initiatives
Moreover, the initiative must be seen in the context of increasing pressure on donor countries’ public finances and the significant savings already made in international cooperation. If this Agenda is ultimately no more than a means of mitigating austerity programs at the expense of other health initiatives, its overall impact on global health could be extremely serious.
In addition, the document stresses the crucial role of domestic resource mobilization in achieving the CSU. This is an undeniable truth. However, the way forward for increasing domestic funding remains unclear. In Africa, for example, the Abuja Declaration (2001), in which governments pledged to devote 15% of their national budgets to health, set targets that the majority of African countries have yet to reach. Even when the GDP of African countries is doing well, this does not systematically translate into increased public spending on health. For example, between 2001 and 2015, public spending on health as a percentage of total expenditure fell in 21 African countries.
Many developing countries face weak tax collection systems and limited economic resources. The Agenda must be accompanied by concrete strategies to strengthen domestic resource mobilization, possibly through innovative financing mechanisms such as debt swaps or levies on international financial transactions. In addition, the international community must meet its commitment to increase Official Development Assistance (ODA) for health, particularly for low-income countries.
Accountability, transparency and inclusion
The success of the Lusaka Agenda hinges on strong accountability mechanisms. The document emphasizes the need for mutual accountability between all stakeholders – donors, recipient countries, civil society organizations (CSOs) and communities. However, details on how this accountability will be implemented are scarce.
Despite the detailed roadmap presented in the “next steps” document, many questions remain as to the primary role of government entities in the realization of the Lusaka Agenda. Striking the right balance between government involvement and the space given to civil society organizations (CSOs) and communities remains a major challenge.
Clear and measurable benchmarks need to be established to monitor progress towards agreed changes. Transparent reporting mechanisms are essential to ensure that all actors are held accountable for their commitments. In addition, promoting a culture of open data sharing is crucial for informed decision-making and course correction where necessary.
Conclusion: Pessimism of reason or optimism of will?
The Lusaka Agenda forces us to face up to the limitations of the current system and the likely failure of the 2030 global health goals. However, if we are to realize the “new perspective” it advocates, we need to go beyond rhetoric and draw up concrete action plans with measurable milestones. In reality, the real challenge lies in implementation. All in all, only time will tell whether it ushers in a new era of collaboration and gives countries, particularly in Africa, the means to achieve the goal of universal healthcare for all their citizens.
If the past can sometimes nourish a pessimistic sentiment, the need to act calls on us to cultivate a deliberate optimism. In other words, despite the uncertainties surrounding this initiative’s chances of success, we must never give up. The lives of millions of people are at stake.
