
Sustaining Sustainability: On the Agenda of the 51st Global Fund Board meeting
Author:
Ekelru Jessica et Christian Djoko
Article Type:Article Number: 2
This article provides an in-depth overview of the main points and discussions surrounding the Sustainability report presented to the Board members during the 51st Board meeting of the Global Fund, held in Geneva from April 22 to 24, 2024.
Context
At the 51st meeting of the Global Fund Board, held in Geneva from 22 to 24 April 2024, a report on sustainability issues was presented. It provides an overview of the current context of discussions and actions on sustainability governance; highlighting the changing health and economic landscape, focusing on progress in health, the challenges faced by poor and vulnerable populations, and emerging barriers.
The challenges of a changing world
The tussle of competing priorities: The COVID-19 pandemic, a seismic shockwave that swept the world, is a stark reminder of our continuing vulnerability to unforeseen health crises. In addition, the successes achieved in the fight against HIV, tuberculosis and malaria (HTM) have been accompanied by an increase in the number of non-communicable diseases (NCDs). This inexorable rise in NCDs – such as diabetes, heart disease and cancer – is creating a multi-faceted arena for global health. While the eradication of HIV/AIDS, tuberculosis and malaria remains a major health priority, the management of the other diseases mentioned above represents a major challenge for the Global Fund in terms of resource mobilisation.
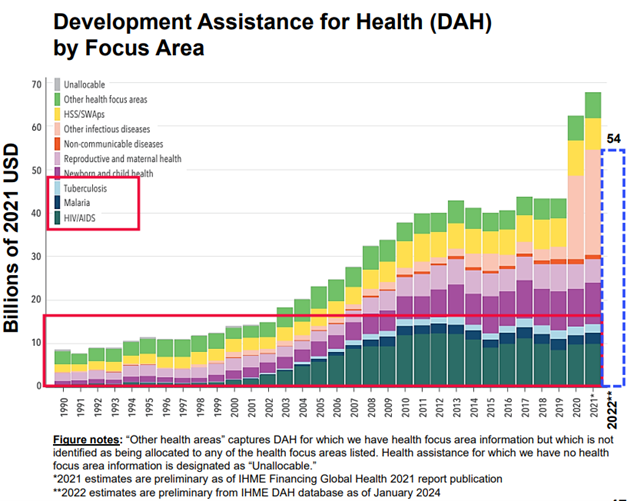
Increased vulnerability and fragility in protection from diseases for certain populations: in an increasingly turbulent world, the security and well-being of the most marginalized and vulnerable populations are under threat (Figure 1). Regressive movements opposing human rights and gender equality are gaining ground around the world, as evidenced by both policy changes and concrete actions. Meanwhile, the space for civil society to defend these fundamental rights is shrinking, further exacerbating the challenges faced by those already on the margins.
Figure 1: Threats to security and well-being of the marginalized
As conflicts intensify around the world, the number of people displaced within their own countries or forced to seek refuge abroad is also increasing. This influx of displaced people is putting immense pressure on already strained health systems and disease control programs, threatening to undermine progress made in the fight against prevalent diseases.
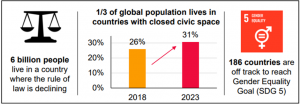
Growing fragility, which mainly affects those living in extreme poverty, is in reality a complex problem fuelled by a variety of economic, environmental, human, political, security and societal factors (Figure 2).
Figure 2: The drivers of fragility
In 2022, fragile contexts affected a quarter (24%) of the world’s population but had a considerable impact on three quarters (73%) of people living in extreme poverty around the world. By 2030, this proportion is expected to increase to include up to 86% of people living in extreme poverty worldwide.
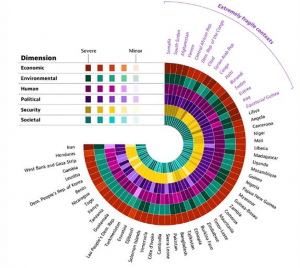
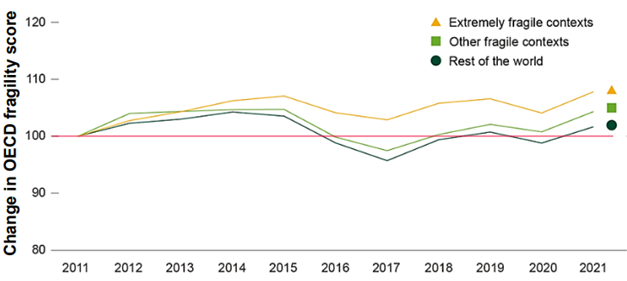
The report presented to the Board notes that 14 of the 15 countries classified as extremely fragile by the international Organization for Economic Cooperation and Development (OECD) (Figure 3) are also designated as COE countries (Challenging Operating Environment) by the Global Fund. Although COE s represent only around 16% of the world’s population, they are home to a significant proportion of refugees, accounting for 87% of asylum seekers and refugees, and 41% of internally displaced people worldwide.
Figure 3: Change in OECD Fragility Score for Countries
Climate change: Climate change acts as a threat multiplier, exacerbating existing vulnerabilities and complicating the fight against HIV/AIDS, tuberculosis, and malaria. More frequent and intense extreme weather events disrupt health services, damage infrastructure, and displace populations (Figure 4), often the most vulnerable. Rising temperatures create favourable conditions for mosquito breeding, potentially increasing malaria transmission rates. In addition, climate change can trigger food insecurity and malnutrition, weakening people’s immune systems and making them more susceptible to infectious diseases such as HIV and tuberculosis.
Figure 4: Internal Displacement due to Climate Change
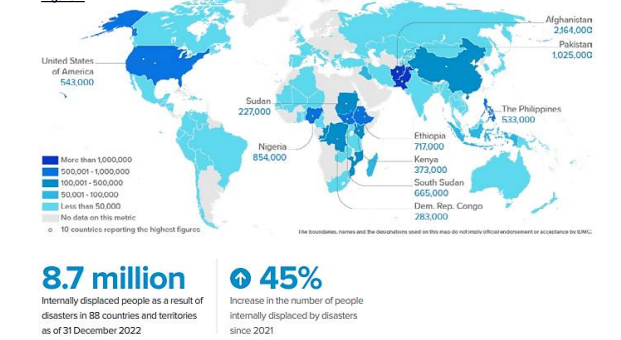
Demographic change also poses a challenge. Rapid urbanisation can lead to overcrowded living conditions, facilitating the spread of infectious diseases. Ageing populations are more likely to develop complications from tuberculosis and may require different approaches to treatment. In addition, the rise of NCDs such as diabetes and heart disease can interact with HIV/AIDS, TB and malaria infections, creating complex treatment challenges.
The emergence of drug-resistant strains of HIV, tuberculosis and malaria is also a growing concern. Inappropriate use of antibiotics and antivirals can accelerate the development of resistance, potentially rendering current treatments ineffective. This requires ongoing research and development of new drugs and diagnostics, as well as robust surveillance systems to monitor the emergence of resistance and adapt treatment regimens accordingly.
Health challenges: The pursuit of Universal Health Coverage (UHC) remains a crucial global objective, but recent assessments indicate that significant challenges remain in achieving goal 3.8 of the Sustainable Development Goals (SDGs) for UHC. Despite efforts to strengthen health systems in line with UHC targets, it is widely recognised that more work is needed to close the gap between current progress and the UHC targets of the SDGs.
A significant contributing factor to the challenges faced in achieving the UHC goals and, more broadly, in strengthening health systems and disease control programs (HIV, tuberculosis, malaria) is the reduced scope for domestic health financing. Indeed, many low-income countries (LICs) and middle-income countries (MICs) are struggling with escalating debt burdens, due to factors such as rising interest rates and inflation. The proportion of LICs and MICs experiencing or at high risk of debt difficulties has doubled over the past decade, placing significant constraints on governments’ ability to allocate resources to health programs and strengthen health systems.
The negative impact of the COVID-19 pandemic has exacerbated these challenges. Whereas before the pandemic, some countries were experiencing relatively stable growth in public spending on health until 2021, the health crisis has significantly disrupted these trajectories. This disruption has been so profound that many countries, including 48 LICs and MICs, do not expect to return to pre-pandemic levels of healthcare spending before 2027, or even later. This has direct implications for global health outcomes, underlining the scale of the pandemic’s impact on healthcare systems worldwide.
An uncertain economic landscape: Amidst the current global economic landscape, there is a sense of cautious optimism. Global growth projections have shown a slight improvement, supported by the unexpected resilience shown by the US and several major emerging and developing economies. In addition, the fiscal support measures implemented in China have contributed to this positive outlook.
However, it is important to note that forecasts for the years 2024-25 remain below the historical average growth rate of 3.8% recorded between 2000 and 2019. Although there are signs of recovery, the global economy has not yet fully returned to pre-pandemic levels of growth and stability.
In terms of Official Development Assistance (ODA), there was a notable peak in 2022. ODA reached a record level of US$218 billion during this period, marking a significant increase of 17% on the previous year. However, it is essential to emphasise that this increase in ODA can mainly be attributed to the rising costs of refugees in donor countries, totalling US$32 billion, and a substantial increase in aid to Ukraine, amounting to US$18 billion (Figure 5). While this demonstrates a commendable commitment to addressing urgent global challenges, it also highlights that priorities have shifted to resolving conflicts and humanitarian crises. There remains, therefore, a continuing need for sustained and diversified efforts to support long-term development goals across diverse regions and sectors.
Figure 5: Official Development Assistance Trend
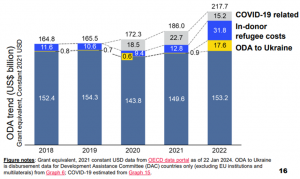
The Global Fund’s current response to sustainability challenges
The Global Fund faces a diversity of sustainability challenges across its portfolio, although some common elements emerge. The sustainability of health programs is influenced by many key factors, varying from country to country and requiring responses tailored to each context (Figure 6).
Figure 6: Key Factors and Levers in Global Fund Sustainability
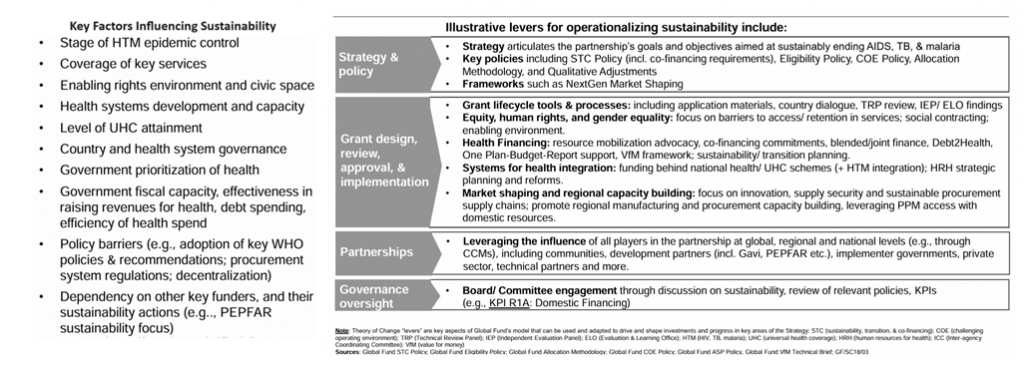
The Global Fund’s key policy tools for addressing these issues, include eligibility policy, allocation methodology, and the Sustainability, Transition and Co-Financing Policy (Figure 7).
Figure 7: Global Fund Policies to Support Programmatic Sustainability
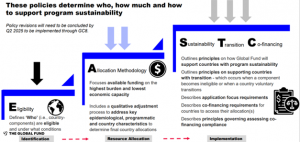
The Global Fund’s eligibility policy covers 126 countries, 87 of which are expected to remain eligible until 2040. Transitional funding is provided when a component becomes ineligible, except in the case of a transition to high income status.
At the last review in 2021/2022, Gross National Income per capita (GNI p.c.) was confirmed as the main eligibility criterion, with some minor adjustments for malaria and exceptions for small Upper Middle-Income economies (UMICs). For the eighth replenishment cycle (GC8), a revision of the disease burden metrics for UMICs is proposed, in parallel with the burden indicators of the allocation methodology but it is noted that this may not generate significant savings, as these countries generally receive small and targeted allocations. The Strategy Committee will examine any updates to the eligibility policy, which would need to be progressive to facilitate responsible transitions for more UMICs However, this could potentially reduce the influence of the Global Fund in these contexts.
A review of the allocation methodology (see A Brave New Method in the Offing?) is already underway, ensuring its robustness under different funding scenarios, including lower levels of funding. Currently, allocations prioritise the provision of more funding to LICs through the Country Economic Capacity (CEC) curve. This curve will be reviewed to determine whether further adjustments are required. In addition, in order to prepare for possible lower funding scenarios, more targeted approaches will be explored. This may include consideration of allocation reductions for MICs with strong sustainability plans, capacity and commitments, while carefully weighing the trade-offs involved.
Furthermore, the report submitted to the Board highlights that there are significant sustainability challenges regarding investments in resilient and sustainable systems for health (RSSH) in the context of GC8, particularly with the end of funding for the COVID-19 Response Mechanism (C19RM) in December 2025. In this context, catalytic investments for GC8 represent an opportunity to target priority areas to effectively address existing challenges. This strategic approach aims to ensure sufficient funding for country allocations while maximising impact and sustainability.
About the Global Fund’s Sustainability, Transition and Co-financing (STC) policy, the report highlights several key points. First, it stresses the importance of national health strategies, health financing, national strategic plans to guide health interventions and the efficient allocation of resources and the use of national systems for the implementation of health programs to strengthen the sustainability and effectiveness of health interventions at country level.
The policy emphasises the need to target key populations and overcome structural barriers to health, to ensure equitable access to health services for marginalised and vulnerable groups. It also encourages countries to identify efficiencies and optimize their disease control strategies to maximise the impact of health interventions.
In addition, the policy encourages additional national investments in health and the application of progressive co-financing conditions to encourage countries to take ownership of their health programs and invest in their sustainability. The Global Fund is also working with its partners to advocate for programmatic and financial changes that support sustainable health interventions.
Regarding transition, the policy defines clear objectives and commitments. It supports country readiness for transition, encourages inclusive assessments of transition readiness and develops transition work plans. The Global Fund also allocates transition funds to countries that become ineligible and provides annual transition projections to facilitate planning and predictability for countries in transition.
Stakeholder Feedback
Stakeholders broadly welcomed the high-level contextual framing and overview of the Global Fund’s multifaceted approach to sustainability. However, concerns were expressed about the political and financial landscapes, which could pose significant challenges to the sustainability of health programs. There was consensus on the need for a strategic approach to address these challenges and ensure the continuity of healthcare services.
Stakeholders emphasized the importance of developing sound national health strategies and financial plans that consider the unique circumstances and challenges faced by each country. Indeed, the country case studies (Colombia, Niger, Malawi, Kenya, Indonesia) highlighted the specificity of sustainability challenges in different contexts, underlining the importance of the flexibility of the Global Fund’s policy framework and its sustainability levers to adapt effective approaches to different contexts.
It is emphasized that sustainability priorities must be defined at national level, with intensified support for the most burdened countries and those closest to transition. It is also recommended that sustainability efforts be aligned with national approaches and harmonized with other development partners. Sustainability efforts in areas where the Global Fund has a comparative advantage, such as pooled procurement, co-financing, and transparency of health financing data, are encouraged.
In addition, discussions highlighted the importance of striking a balance between financial sustainability and programmatic efficiency. It was recognized that sustainable health gains can only be achieved through the development of mechanisms that reduce reliance on ongoing external funding while ensuring the continued delivery of essential health services.
Improvements in grant-making tools, equity, gender and human rights approaches, as well as the expansion of health financing expertise within the Secretariat, have already addressed many sustainability challenges. Health systems strengthening is identified as one of the most important levers for improving sustainability, with a particular focus on collaboration with other organizations on health systems strengthening.
Regarding allocation, eligibility and STC policies, it is emphasized that the Global Fund’s current policies have served its purpose well, effectively channelling funds to the poorest and most disease-affected countries. Therefore, a significant reduction in country eligibility for the Global Fund is not recommended, as this would risk undermining progress in reducing the disease burden and threaten human rights-based approaches.
Conclusion
Looking to the future, stakeholders stressed the importance of developing clear, actionable plans that incorporate feedback and real-life experiences from countries facing sustainability challenges. There was shared agreement on the need for ongoing dialogue and adaptation of strategies to changing circumstances to effectively address these challenges.
