
Looking ahead to implementing the Global Fund Strategy in Grant Cycle 7: Part I
Author:
Aidspan
Article Type:Article Number: 6
Global Fund Board considers progress in HTM under GC7
This is the first of three articles on Looking ahead to Grant Cycle 7 – Strategy, in which we examine the Strategy’s “Primary Goal – HIV, TB and malaria”. It is based on a presentation to last month’s Board meeting and sought Board feedback to encourage more strategic and holistic discussions.
When the Board met last month in Geneva, the Secretariat presented a status report on current progress towards the Global Fund mission and Strategy as it enters the Grant Cycle 7 (GC7) funding period.
The paper was based on the work of the Board’s Committees’ (Audit & Finance (AFC), Ethics & Governance (EGC), and Strategy [SC) meetings in October, highlighting important areas with “in-depth analysis and candour” (says the report) where the Secretariat specifically wants the Board’s engagement and leadership.
In particular, the Secretariat wanted the Board to review the overarching data on its collective achievements and the work remaining with the following questions in mind:
- Are there observations on the preparations and/or preliminary findings from GC7 from member constituencies that are not captured here?
- Where can the organization mobilize the broader partnership (including member constituencies) to address implementation challenges?
- How can the partnership leverage and evolve what its collectively built to continue to deliver results in a changing global context?
The presentation was in four parts:
- Looking ahead to Grant Cycle 7 – Strategy: Primary Goal: HIV, TB and malaria.
- Looking ahead to Grant Cycle 7 – Strategy: Mutually reinforcing contributory and evolving objectives: Community, rights and gender (CRG).
- Looking ahead to Grant Cycle 7 – Strategy: Mutually reinforcing contributory and evolving objectives (continued): RSSH/PP/C19RM/Health Financing.
- Looking ahead to Grant Cycle 7 – Strategy: Mutually reinforcing contributory and evolving objectives (continued): Unique strengths of Global Fund (including Market Shaping) and Discussion on Future
This and our next two articles summarize the presentations.
Setting the scene
- At the close of 2023 the Global Fund will have approved more funding than any other year in its history. This is an immense responsibility and opportunity for the partnership. The Strategy charts the way the partnership invests to end HIV, TB and malaria, while building resilient systems for health prepared to respond to emerging pandemics and keeping people and communities at the center. This session focused on a holistic overview of the status of Strategy implementation as the Global Fund launched GC7, building from detailed discussions at Committee meetings.
- There are interdependencies at the country and regional levels (political, programmatic, financial) that can exceed the influence and reach of the Secretariat, particularly during implementation. To be successful in GC7 and beyond, the Fund needs the entire partnership. This integrated update highlights progress to global goals with work remaining ahead of 2030; preparation to maximize GC7 investments; and preliminary observations from the funding requests themselves.
- While the key performance indicators (KPIs) reflect the strength of collective efforts and aspects of historic progress, the work is not done. The Global Fund does not exist outside a coordinated global anti-rights movement in which key and vulnerable populations face increasingly hostile political rhetoric, crackdowns on their activities, and restrictions on civic space that are putting them and their work at risk. Nor is the Global Fund immune from multi-crises ranging from debt to conflict to climate change affecting the world in which it operates. Less solidarity and increased discrimination will result in greater health inequities going forward, putting at risk the shared aspirations for Universal Health Coverage (UHC) – particularly the “U”.
- This is a time for renewed collective action without which the world is at severe risk of failing to achieve Sustainable Development Goal (SDG) targets for health. The Fund asserts that “we must seize this opportunity of unprecedented investment to end HIV, TB and malaria’s devastating impacts; to dramatically strengthen integrated health and community systems and their resiliency to prepare and respond to the next pandemic; and to get closer to all aspects of UHC, through access for all to the best treatments at the lowest costs, even in the most challenging contexts. This is what the Global Fund can accelerate in GC7, but we cannot do it alone”.

While some countries are reaching HIV epidemic control, the global targets are off track
There has been very strong progress on reducing AIDS-related deaths in countries supported by the Global Fund. However, in 2022, there were 507,000 deaths globally due to AIDS-related causes. Progress is mixed, varying significantly between regions.
New HIV infections are at their lowest in decades but we are still off track to meet global target. Progress by geography is mixed. The most significant reductions in new HIV infections were in sub-Saharan Africa (SSA). Beyond SSA, reductions have been modest and/or variable with alarming increases in new infections in some regions like Eastern Europe and Central Asia.
Despite important progress, significant efforts are needed in most regions to reach the UNAIDS 2025 AIDS targets
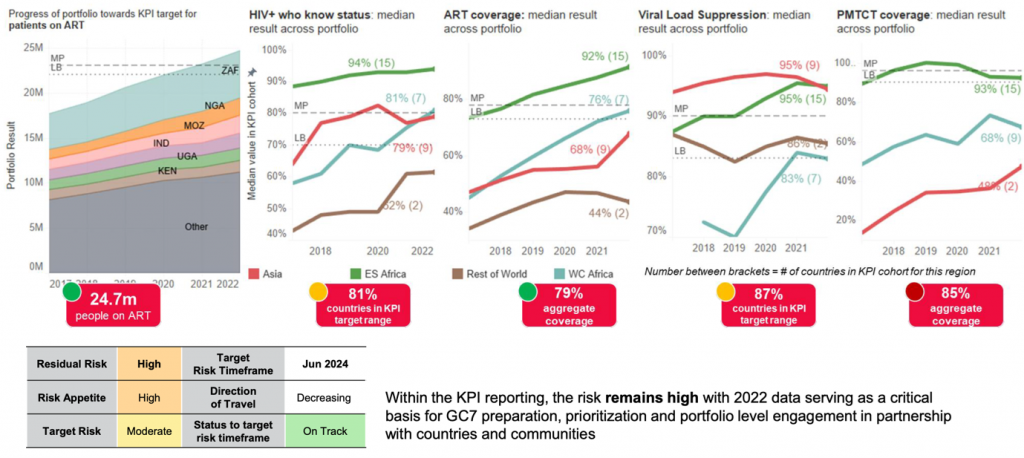
Source: https://aidstargets2025.unaids.org/
Coverage of HIV prevention programs for KPs is sub-optimal, as new infections continue to rise
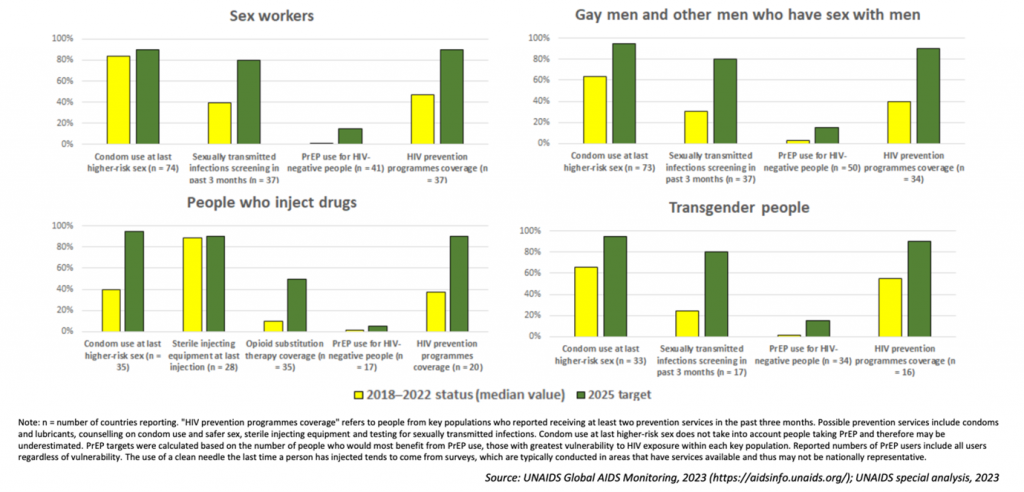
GC7 preparation focused on increasing access and greater HIV impact

HIV Program Essentials in FRs indicate implementation barriers and distance between policy and practice
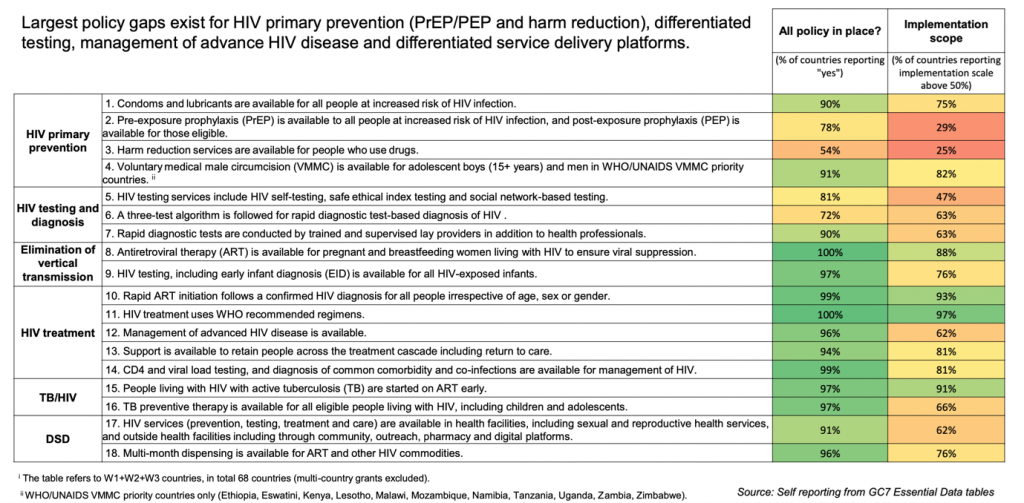
Early observations on GC7 plans and ambitions highlight that preparation had an impact, but gaps remain
On the plus side:
- Program Essentials helped to focus country dialogue and identify missing or lagging implementation.
- Greater use of HIV incidence data to prioritize HIV prevention investments (priority geographies and sub-populations).
- Increased focus on high impact HIV prevention interventions, including greater ambition for PrEP, needle and syringe programs and condom programs.
- Progress on transition to dolutegravir-based regimens (>80% of people on antiretroviral therapy (ART) use DTG-containing regimens in GC7 FRs to date) – and optimization of HIV products, e.g., more HIV duo tests.
- Significant price reductions for HIV first line antiretroviral drugs (ARVs) and some diagnostics (e.g., TLD <$45 per person, per year for the first time – a 25% reduction; blood-based HIV self-tests now available at $1).
- Increased investment in sexual and reproductive health (SRH), co-infections and co-morbidities.
- Matching Funds have catalyzed ambition including for PrEP and greater scale of HIV prevention for key populations.
On the minus side:
- Significant gaps for ART/advanced HIV disease, condoms and PrEP identified in gap tables and prioritized above allocation request (PAAR).
- HIV prevention coverage gaps continue.
- Many applicants faced significant prioritization challenges (see Technical Review Panel (TRP) Windows 1, 2 and 3 reports).
Looking ahead for HIV
Collective action is needed to address the challenges –not easy to do so but nonetheless possible.
Outstanding challenges
- Delivering quality, tailored prevention programs at scale remains a challenge, exacerbated by stigma, discrimination and closing civic space.
- The reach of HIV prevention programming for people with significant prevention needs is insufficient for impact (especially young KPs) – compounded by challenges in KP size estimation.
- Financing remains a challenge – domestic contributions have not increased to offset slight decline in external funding in real-terms.
- Sustainability (and fragility) of the HIV response is a critical concern for countries approaching epidemic control.
- U = U – maintaining lifelong viral suppression for large cohorts is necessary to sustain lower incidence – but is a challenge in terms of costs and quality of services.
- Strengthened cross-sectoral collaboration is needed to improve integration to meet evolving needs of people living with HIV (PLHIV) and affected communities (significant comorbidities/coinfections impacting on health outcomes).
- Prioritization is difficult, but needs strengthened focus to increase impact and Value for Money (VfM).
Actions for Secretariat and Partnership
- Leverage lessons learned to date to strengthen focus of remaining GC7 FRs and to support national programs, including:
- Catalyze greater integration of HIV services within comprehensive packages of essential services.
- Expand service delivery options (e.g., pharmacies, bars), especially for prevention and testing. Invest in ‘last mile’ service delivery.
- Invest in national and regional public health institutions (including regulatory capacity).
- Continue to invest in data for impact, including for size estimations of KP and adolescent girls and young women (AGYW) subgroups.
- Harness demographic and digital transformations.
- Integrate successful investment approaches generated by GC6 catalytic investment in differentiated service delivery (DSD), condom programs, TP, HIV prevention for AGYW and human rights.
- Focus on policy, program, financing and systems shifts needed to underpin the sustainability of the response.
- Continue coordination with technical partners to support the prioritization of high impact interventions (including program essentials).
- Continue efforts to ensure more affordable, accessible and long-lasting HIV products.
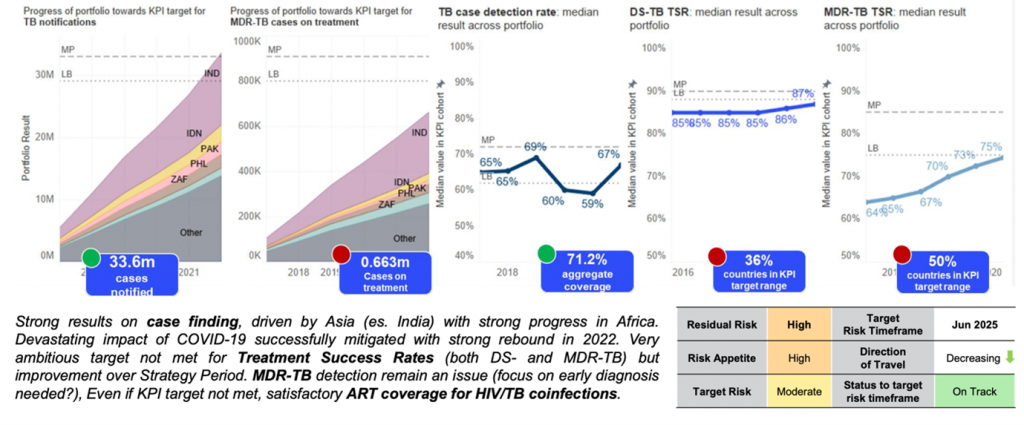
While there was a rebound in 2022, global targets remain off track
The disruption of COVID-19 on TB services was severe and the estimated 10.6 million people with TB in 2021 increased 4.5% from 2020 and 1.6 million people died from TB (including 187,000 HIV positive people). Preliminary data from 2022 indicates a rebound from COVID-19, and while C19RM allowed for additional investment of $400 million, there is a significant funding gap to reach END-TB targets.
Within KPI results, despite strong case finding, treatment success and MDR-TB require urgent attention
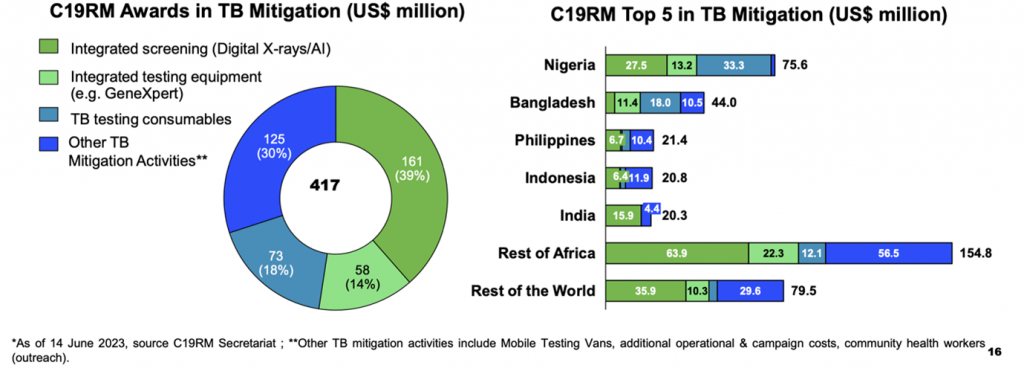
C19RM was critical for TB recovery
A total of $417 million has been awarded to TB mitigation and Integrated testing. Requests for integrated screening and testing are generally submitted and awarded under the TB mitigation category, while contributing to strengthening multi-disease lab systems and diagnostics networks.
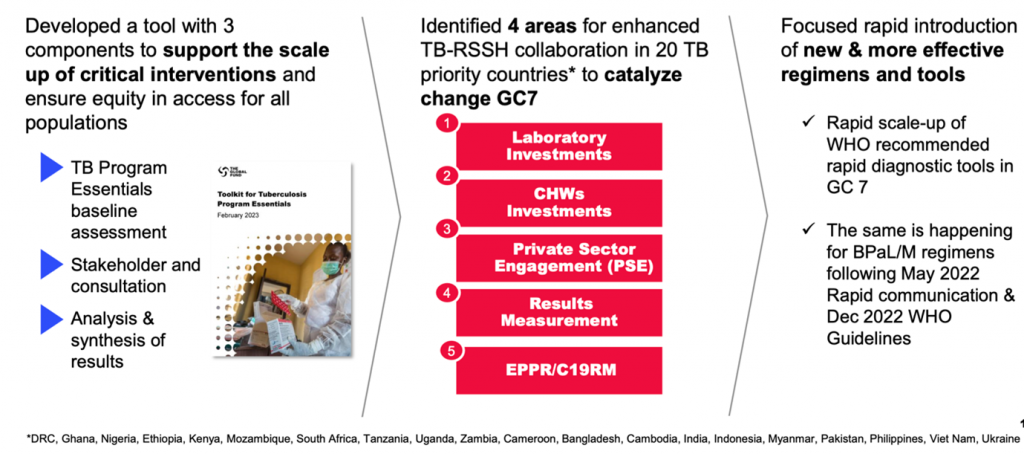
GC7 preparations introduced Program Essentials, prioritized RSSH/PPR collaboration to catalyze change & rapid introduction of new tools and regimens
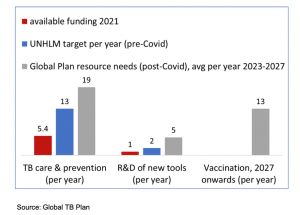
Despite price reductions in key TB commodities, there is a significant funding gap in essential commodities in GC7
- The Bedaquiline price drop from $289 for a six-month (6M) course to $130 per 6M course from Lupin: $194 per 6M course from Janssen was announced at the end of August.
- 30% price decrease for 3HP (TPT) from $15 to $10.
- 20% price decrease for Xpert Cartridges taking the Xpert Ultra cartridge from $9.98 to $7.97. The agreement also has commitments on Service & Maintenance of machines. The Xpert XDR cartridge remains at $15.
What this means and ongoing actions
✓ The funding gap for the 54 countries which submitted FRs in W 1-3 is $1 billion. The gap is largely comprised of essential commodities, especially diagnostics.
✓ Incorporating efficiency into the grant making process should increase coverage of these and other TB commodities. Efficiencies will also trigger essential commodities to be moved from the PAAR.
✓ Global Fund will continue to work with partners to shape the market for other TB essential commodities and further price reductions.
✓ Global Fund will work with partners for innovative financing and with countries to increase domestic funding.
✓ Cross cutting TB interventions integrated into RSSH and C19RM .
Looking ahead post-UN High-level Meeting (HLM), advocacy and resource mobilization will be key to ending TB
Outstanding challenges
Actions for Secretariat and Partnership
Secretariat: Maintain focus on scaling up innovations in screening, diagnostics, treatment and prevention while accelerating Nextgen of products (e.g. antigen-based skin tests; LF-LAM technologies; next generation mWRD; paediatric formulations; TB vaccines); collaborate on RSSH catalytic investments in laboratory, community health workers (CHW); PSE; and increasing measurement.
Integrating technical assistance for DR-TB into the grants, building from the support provided through Green Light Committees.
Larger partnership considerations:
- Urgent need to ramp up funding for TB programs, increasing domestic funding, supporting innovative financing mechanisms.
- Investing in TB strengthens pandemic preparedness. Fighting today’s pandemics builds country capacity to fight the next pandemic.
- Scale-up equity and access to innovations to accelerate our progress toward ending TB.
- The three UNHLMs on health this year and HLM on AMR in 2024 provide an opportunity to foster greater integration of efforts to end the major pandemics of today like TB, to enhance pandemic preparedness, tackle antimicrobial resistance and to make progress toward UHC.

We are off track on Global Technical Strategy for Malaria
By 2020, key milestones for reducing malaria cases and deaths had not been achieved, but milestones for elimination and prevention of reestablishment had been met. By 2021, global malaria case incidence was 59 cases per 1,000 population at risk, against a target of 31 cases per 1,000 – off track by 48%
KPI results remain low with a recent increase to very high risk
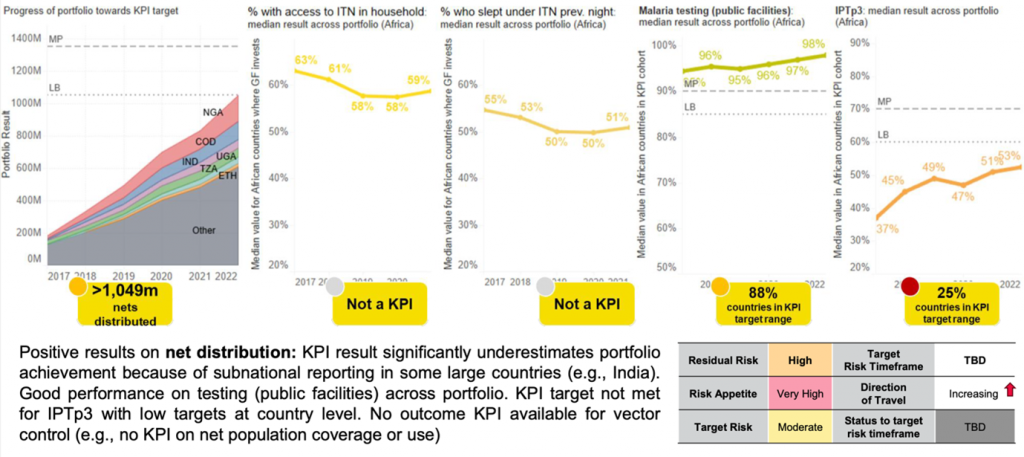
Threats to ending malaria are real and here now, but some are looming
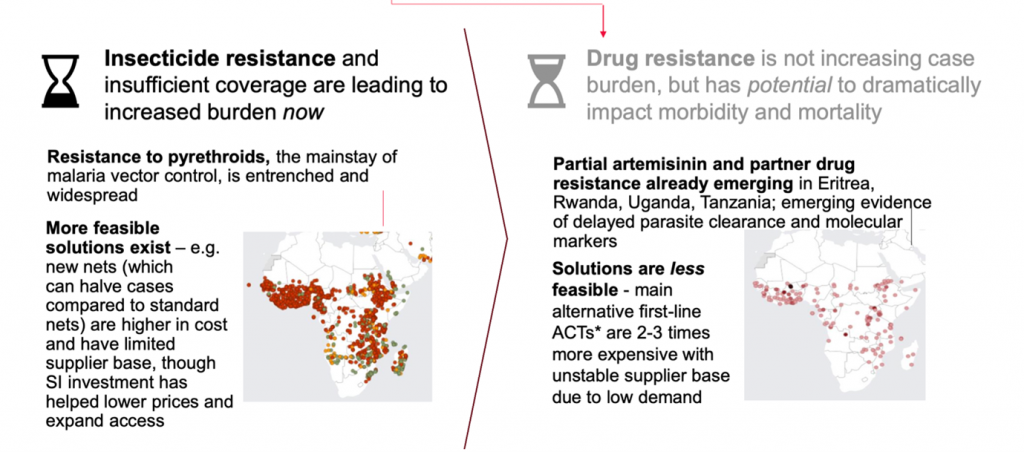
Four thematic challenges
- Financial gaps – we don’t have enough money. So, for example, even as the quality of programming is improving and more cost-effective, there’s a higher absolute cost.
- Insecticide resistance – our tools are not as effective as they used to be and we need to act with urgency. In GC6, the Global Fund along with other partners used catalytic investments to bring tools faster and mainstream, driving down costs, but funds to drive change are constrained in GC7.
- Climate change – the disasters and events disproportionately impact malaria (malaria grants accounted for 45% of the Emergency Fund utilization in GC6).
- Health systems – early diagnosis and treatment coupled with timely and accurate reporting and recording is critical to drive quality malaria care as an essential part of basic primary health services
Themes emerging based on preliminary analysis of Windows 1 and 2, particularly funding gaps
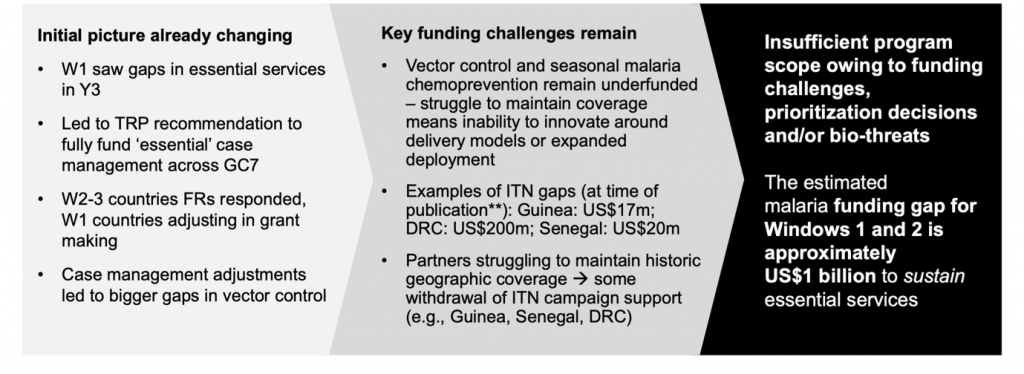

In the longer term, we need different levers (including some in the pipeline) and evolved approaches
- Exploring innovative financing approaches is critical as the funding gaps require increased capital beyond domestic, partner and GF resources. This may involve trade-offs within how we allocate funding to malaria as the GF; all options need to be investigated.
- Improving effective vector control is essential to maximize the impact of our most important tools
- Preparing for drug resistance should not be a choice given early indications of resistance – investment in new treatments now ensures we can respond to a tipping point
- Ensuring the new vaccines are appropriately prioritized given limitations to their incremental cost effectiveness
- Building RSSH with an emphasis on primary health care must be part of the global plan. These will be critical with climate change realities upon us.
******
Board paper GF/B50/08 Strategy Implementation: Acceleration into Grant Cycle 7 will soon be available on the Global Fund website.
