
A third of Cameroonians do not use their mosquito nets
Author:
Julien Chongwang
Article Type:Article Number: 9
For a variety of reasons, 32% of people in Cameroon prefer not to use their mosquito nets to prevent malaria. This situation is hindering the fight against this disease, which still claims thousands of victims every year.
In a press kit published to mark World Malaria Day 2023, Cameroon’s Ministry of Public Health, through the National Malaria Control Programme (NMCP), suggested that almost a third of people in the country do not use the mosquito nets that they have received for malaria prevention. “It should be noted, however, that only 68% of people who have long-acting impregnated mosquito nets (LLINs) actually use them,” says the report.
The press kit provides no further details. But for Raymond Tabué, head of the Integrated Vector Control Unit at the NMCP, the primary explanation lies in people’s poor understanding of the usefulness of mosquito nets. “Lack of awareness of the importance of the mosquito net or its usefulness in preventing malaria remains a barrier to the use of this tool”, he said.
In his opinion, educational level may be one factor, as well as the level of knowledge being higher in urban than rural areas: “You will find that the further you are from the city, the less knowledge you come across”.
But beyond this ignorance, sociological and anthropological considerations are partly responsible for many Cameroonians’ refusal to use mosquito nets According to Tabué, research to date has noted that some people complain about feeling uncomfortable when they are under the net. “Some people say that they feel suffocated when they are under a mosquito net, while others mention the skin irritation that contact with the net could cause because of the insecticide it contains”, reports Raymond Tabué.
He goes on to say that others cite aesthetic reasons, for example, that installing a mosquito net will damage the walls of their rooms. In residential areas, he says, very few houses have installed mosquito nets. In fact, to avoid hammering nails into their walls or ceilings, residents often prefer to install window screens to keep out mosquitoes.
Raymond Tabué ends his list of causes by saying that “in the northern part of the country, the mosquito net, which is generally white, is associated with the funeral shroud; hence many people don’t want to use something of this colour. In war zones, where people are on the move a lot, the rectangular mosquito net is no longer very suitable; people prefer a cone-shaped net”.
Survey results
A survey conducted in the northern provinces of Nord and Extrême-Nord and published in 2020 under the title ” Survey on the determinants of malaria-related behaviour” (in French only) confirms many of the behaviours mentioned by Raymond Tabué.
It states that “some negative attitudes towards mosquito nets are common. For example, 44.8% of people surveyed said that they did not like sleeping under a mosquito net when it is hot (…) and 39.1% said that the insecticide in mosquito nets bothered them”.
The survey, carried out by Breakthrough Action, a structure based at the Johns Hopkins Center for Communication Programs in the United States, also mentions that “the number of people who feel that sleeping under a mosquito net every night is problematic because of the difficulty of unfolding it is higher in the North (27%) than in the Far North (18.4%)”.
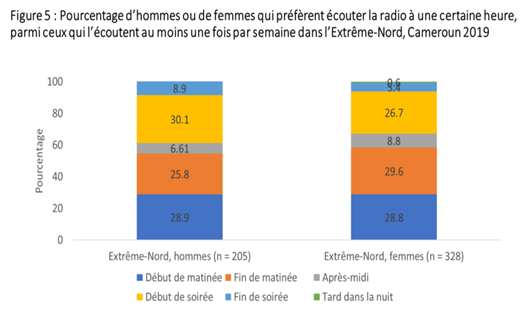
Source : https://malariabehaviorsurvey.org/wp-content/uploads/2021/11/CAM-MBS-Report-2019-Fr.pdf (p. 32).
Above all, however, the study found that “attitudes towards mosquito nets are generally positive among those surveyed. More than nine-tenths of those surveyed believe that it is easier to have a good night’s sleep when sleeping under a net (90.6%) and that nets are useful (95.6%)”.
Be that as it may, the refusal to use mosquito nets by large sections of the population is not unique to Cameroon. Citing the World Malaria Report 2022 Margaret Reilly McDonnell, Executive Director of United to Beat Malaria, regrets that “net use in sub-Saharan Africa has fallen slightly since peaking in 2017”.
Yet, she says, mosquito nets play an “essential” role in the fight against malaria. “The World Health Organization (WHO) has estimated that mosquito nets have prevented 1.3 billion cases of malaria and 6.8 million deaths from the disease since 2000, and a 2015 study in Nature estimated that mosquito nets were responsible for 68% of all malaria cases prevented between 2000 and 2015,” insists Margaret Reilly McDonnell.
Raising awareness
To underline the impact this situation may have on the fight against the disease, she draws attention to the fact that between 2016 and 2021, reported malaria deaths in Cameroon increased by 43%, from 2,639 to 3,872. Most of these deaths involved children under the age of five.
“Consider the long-term impact, not only on families and communities, but also on Cameroon’s economy. These are not just lives; these are future doctors, lawyers, community leaders”, says Margaret Reilly McDonnell.
As a result, experts recommend stepping up awareness-raising campaigns to bring about a change in people’s behaviour with regard to mosquito nets, using community health workers, churches, mosques and networks of associations to get the message across.
On the other hand, other means of preventing malaria are prescribed in addition to the use of mosquito nets. “I would recommend that communities invest in vector control strategies such as larvicides, spatial repellents to protect you and your family when you are away from the net and join in environmental clean-up efforts to reduce the mosquito population. Removing all standing water from your home and community will have an impact,” says Margaret Reilly McDonnell.
Two other instruments have now been added to this malaria prevention arsenal: chemoprevention of seasonal malaria (CPS) and recently developed and authorized vaccines.
As far as CPS is concerned, a briefing note produced by Médecins sans Frontières (MSF) states that “it consists of administering a combination of anti-malarial drugs – in therapeutic doses – during the season when the risk of malaria transmission is highest”.
“The aim of this action is to reduce malaria-related morbidity and mortality. The drugs recommended for this strategy are a combination of Sulfadoxine-Pirymethamine and Amodiaquine. These drugs take effect approximately 28 days after administration.
According to the World Malaria Report 2022, 15 countries are currently implementing CPS. In these countries, it states, “the average number of children treated per course of CPS has increased steadily, from around 0.2 million in 2012 to nearly 45 million in 2021”.
As far as the vaccine is concerned, since 2021 WHO has recommended the RTS,S, the very first malaria vaccine, which is already being used in certain African countries such as Ghana, Kenya and Malawi where more than 1.2 million children have already been vaccinated, according to WHO data.
Its use will soon be extended to other countries, as some 18 million doses are scheduled to be distributed to 12 countries on the continent between 2023 and 2025.
In addition to RTS,S, a second malaria vaccine is well on the way to being recommended by WHO in the near future. Called R21/Matrix-M and developed by researchers at Oxford University in the UK and the Institut de Recherche en Sciences de la Santé (IRSS) in Burkina Faso, this vaccine is already licensed in Burkina Faso, Ghana and Nigeria.
But, staying with the use of mosquito nets, Raymond Tabué is particularly concerned about the attitude of those who use the nets they receive for other purposes: for example, as goal nets by young footballers, to protect young plants in nurseries, or as window grilles…
And he says: “I think that at some point we need to question the very fact that mosquito nets are distributed free of charge. We have to ask ourselves whether free distribution takes away some of the importance we attach to this tool. Because generally, what is given away for free has very little value”.
In concrete terms, he wonders whether we should not consider socially marketing mosquito nets, even at low cost, knowing that those who buy them will be more likely to actually use them. The downside, however, could be that a number of households would be deprived of this important tool in the fight against this disease.
