
World Malaria Report 2023 paints a gloomy picture
Author:
Christian Djoko
Article Type:Article Number: 3
A worrying decline, according to the World Health Organization
During the COVID-19 pandemic malaria programs were disrupted, leading to an increase in malaria incidence and mortality. Despite the efforts of endemic countries and international stakeholders, these rates remain very high. Five countries have seen the biggest increases, compounded by difficulties such as extreme weather events, conflicts, humanitarian crises, budgetary constraints, biological threats and inequalities which have hampered recovery. Without being overly defeatist, the new World Health Organization 2023 report on the current malaria situation sounds the alarm to redouble our efforts to eliminate malaria as a global public health problem.
The current global malaria picture
The World Health Organization (WHO) new World Malaria Report 2023, paints an alarming picture of the fight against this disease. Globally, the number of malaria cases in 2022 was significantly higher than before the pandemic in 2019: between 2000 and 2019, the number of malaria cases had fallen from 243 million to 233 million. In 2020, a further 11 million cases were reported, with no apparent change in 2021, followed by an increase of five million cases in 2022, bringing the total to almost 249 million cases.
The number of malaria-related deaths in 2022 has also surpassed the pre-pandemic level in 2019. Between 2000 and 2019, these had fallen steadily, from 864,000 to 576,000. Since the start of the COVID-19 pandemic, however, the number of deaths rose by about 10% to an estimated 631,000 in 2020. Despite some marginal decreases over the following two years, the estimated annual number of deaths in 2022 was 608,000, 32,000 more than before the pandemic. Compared with 2019, global malaria mortality remains slightly higher. Malaria mortality, indicating the number of deaths per 100,000 population at risk of malaria, was halved between 2000 and 2019, from 28.8 to 14.1. By 2020, the mortality rate had increased to 15.2, before decreasing slightly to 14.3 by the end of 2022.
Compared with 2019, the incidence of malaria (representing the number of cases per 1,000 inhabitants) worldwide remains slightly higher. Incidence fell from 81 in 2000 to 56.8 in 2019 but by 2020, had increased to 58.7. After a minor fall in 2021, a slight increase was recorded in 2022, bringing the incidence rate down to 58.4.
Five countries – Ethiopia, Nigeria, Pakistan, Papua New Guinea, and Uganda – bore the brunt of new malaria cases worldwide between 2021 and 2022, accounting for most of the five million additional cases observed.
Figure 1. Malaria deaths and cases, globally, 2019-2022
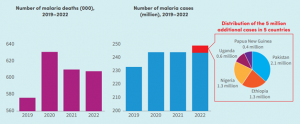
Source: World Malaria Report 2023,
Why is malaria increasing?
Impact of climate change
The link between climate change and the incidence of malaria is closely examined in the Report. Variations in weather patterns can influence the spread of malaria by affecting mosquito habitats and the disease’s transmission. This highlights the importance of considering environmental factors when planning malaria control programs.
More broadly, the Report shows that climate change is a major threat to human health and wellbeing, particularly for the most vulnerable groups. It disrupts natural and man-made systems, affecting the social determinants of health such as livelihoods, nutrition, security and access to quality care. It acts as a standalone separate threat as well as amplifying other threats. Extreme weather events have an impact on health workers and health care infrastructures, particularly in countries with fragile health systems. Vulnerable communities, who have contributed the least to climate change, are the most affected, including women, children, ethnic minorities, the poor, migrants, displaced people, the elderly and those with health problems. Low-income countries and small island developing states suffer the most severe impacts, with mortality rates in vulnerable regions 15 times higher than in less vulnerable regions.
Humanitarian crises and socio-economic threats
During the period 2019 to 2022, 41 malaria-endemic countries faced various health and humanitarian crises, on top of the COVID-19 pandemic. Several experienced significant increases in malaria cases and related deaths, with some even facing epidemics. Ethiopia, for example, has seen a 32% increase in the incidence of malaria due to internal armed conflict. Between 2021 and 2022, the country recorded an increase of 1.3 million cases.
The economic consequences of the COVID-19 pandemic have also exacerbated the impact of malaria, particularly in communities already facing health problems and poverty. In 2020, 70% of low- and middle-income countries affected by malaria experienced a contraction in their economy, with a third of them recording a drop of more than 1% in their gross domestic product (GDP). Although the number of countries experiencing economic difficulties decreased in 2021 and 2022, persistent inequalities in the distribution of wealth are still present in many regions. In addition, economies recovering from recession face the challenges of climate change and diseases such as malaria.
Resistance to drugs and insecticides
WHO is increasingly concerned about the biological threats posed by malaria. The parasites responsible for the disease are developing increasing resistance to first-line drugs such as artemisinin. In addition, mosquitoes, the vectors of malaria, are becoming increasingly insensitive to insecticides, particularly the pyrethroids used on insecticide-impregnated mosquito nets. This resistance is spreading worldwide, with 78 countries confirming that mosquitoes are resistant to at least one class of insecticide. In West Africa, high-intensity resistance to pyrethroids is particularly prevalent. These threats are exacerbated by genetic mutations in malaria parasites which complicate their detection, and by the spread of new parasites and vectors of the disease.
More specifically, the Report highlights that the Anopheles stephensi mosquito, a malaria vector, has spread beyond its natural habitats in Asia and Arabia to reach Africa. First detected in Djibouti in 2012, this mosquito has been associated with several malaria outbreaks. It is difficult to control because of its ability to develop in urban environments, its resistance to extreme temperatures and to many of the insecticides used in public health. Its spread, coupled with rapid urbanization, could increase the risk of malaria in African cities.
Figure 2. Presence of Anopheles stephensi mosquito vector in Africa
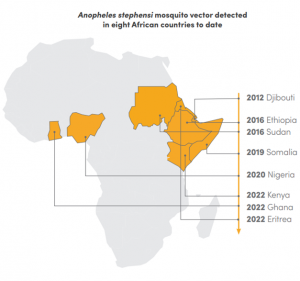
Source: World Malaria Report 2023,
Reasons for hope
Despite this worrying picture, the report underlines the progress made in the fight against malaria since 2000, in particular the reduction in the number of cases and deaths linked to the disease. While progress towards eliminating malaria is showing signs of slowing down in heavily affected countries, says the Report, a growing number of less-affected countries are making progress in eliminating the disease. In 2022, 34 countries recorded fewer than 1,000 malaria cases, compared with just 13 in 2000. Twenty-seven countries reported fewer than 100 cases of malaria in 2022, compared with just six countries in 2000. From 2000 to 2023, 25 countries where malaria was endemic in 2000 reported no cases of indigenous malaria for the third consecutive year, and 15 of them were certified malaria-free by WHO. In 2022, Cabo Verde recorded no cases of malaria for the fourth consecutive year and officially submitted a request for malaria elimination certification, with a decision expected in early 2024.
Figure 3. Decrease in malaria endemic countries between 2000 and 2022
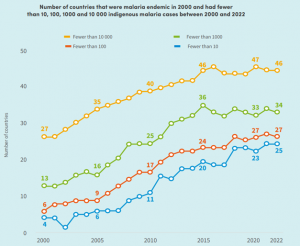
Source: World Malaria Report 2023,
Other successes are also mentioned in the WHO Report, such as the development of malaria vaccines, the availability of new mosquito nets and the intensification of prevention among children at high risk.
The need for further action
The Report concludes by emphasizing that the goal of a malaria-free world is still far from being achieved, and that readjustment is necessary. This implies increased funding, improved tools, data-driven strategies and sustained political commitment. The Report also stresses the importance of comprehensive measures and the mobilization of society to put in place climate-resilient responses to malaria. Finally, it emphasises that the key to mitigating the effects of climate change on malaria lies in sustained efforts to counter global warming, optimize adaptation to climate change and reduce vulnerability.
More specifically, the Report stresses five main levers that need to be operated in order to take effective action against malaria.
- Increasing funding for the fight against malaria
According to WHO data, the global funding gap for malaria control has increased from $2.3 billion in 2018 to $3.7 billion in 2022. Although global spending on malaria control will have reached $4.1 billion by 2023, this is still well short of the $7.8 billion needed to achieve the Global Technical Strategy for Malaria (GTS) targets and the $9.3 billion required by 2025.
The Report also highlights that between 2010 and 2021, on average, 66% of the funds allocated to the fight against malaria came from international sources, with malaria-endemic countries contributing 34%. By 2022, the share of national funding had increased to 38%, while international donors have contributed 62%.
Figure 4. Global and national funding for malaria, 2020-2022
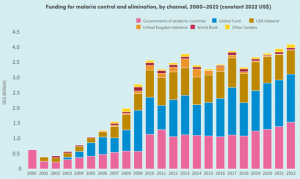
Source: World Malaria Report 2023,
Individuals and households bear most of the financial burden of malaria, with over 47% of households in low- and middle-income countries facing catastrophic health costs in 2020. The financial burden of malaria falls mainly on households, which can restrict access to treatment and exacerbate poverty. This underlines the urgency of implementing universal health coverage and establishing financial protection mechanisms.
- Using information strategically
The Report highlights the importance of robust health surveillance systems and the judicious use of information to assess the malaria burden of disease and develop strategies to control and eliminate the disease. Indeed, the weakness of surveillance, data collection and analysis systems in some countries limits the effective use of this information. Moreover, disparities in capacity between countries are evident, underlining the need for investment to address this. Sub-national adaptations of malaria control interventions rely on local data to determine the appropriate mix of interventions and maximize their impact. WHO says it is supporting more than 30 countries in use of information to apply this approach to decision-making. It is also working on guidelines to help countries prioritize malaria control interventions in the face of imited resources limited resources.
- Leveraging innovation
The WHO Report highlights the importance of investing in new tools to fight malaria. These include effective vaccines, long-acting insecticides, control methods adapted to outdoor bites, single-dose preventive treatments, diagnostics capable of detecting latent stages of infection, new antimalarial drugs and single-dose chemoprevention. It is crucial, says WHO, that these innovations focus on products that are affordable, effective, easy to manufacture and less sensitive to temperature fluctuations. It is also necessary to speed up the marketing process while guaranteeing the quality, efficacy and safety of the products. The international community must support increased supply and reduced costs to facilitate the introduction and development of these new tools. It is also important to strengthen the capacity of the regulatory bodies responsible for assessing and approving these products.
- Strengthening political commitment
Countries must translate their political commitments into tangible resources and actions to save more lives. That said, WHO asserts that it is up to the governments in those countries most affected by malaria to rise to this challenge. Local initiatives that empower people to protect themselves from malaria can foster an environment of accountability and action.
- Ensuring resilient and sustainable malaria services in the face of the threat of climate change
The WHO Report proposes a series of technical and operational measures:
- Speaking with one voice and forging partnerships;
- Decarbonizing healthcare systems and making them more resilient and sustainable in climate and environmental terms;
- Shifting decision-making power from global health institutions to national and community actors;
- Increase knowledge of the link between climate change and health ;
- Optimizing guidelines and tools for health and climate surveillance, monitoring and evaluation;
- Using disease and climate data to make decisions;
- Strengthening detection, preparedness and response to epidemics; and
- Improve national capacity to analyze and use information on malaria and climate, by coordinating training for health and climate professionals.
Conclusion
The World Malaria Report 2023 highlights the continued importance of malaria control as a major global public health threat. It emphasizes the challenges posed by climate change, humanitarian crises, socio-economic threats and drug and insecticide resistance, and calls for concerted action to address these growing threats. Continued investment in malaria control programs, strengthening health systems and ensuring equitable access to prevention and treatment tools are essential to achieving the goal of zero malaria.
