
Redefining strategies to address the multifaceted battle against malaria
Author:
George Njenga Kiai
Article Type:Article Number: 5
The 23rd Strategy Committee discussed an update on malaria which highlighted the complex challenges and strategic pathways in global malaria control amid increasing risks. Despite notable achievements in disease elimination, the persistence of malaria cases underscores the need for a refined, multifaceted approach. The meeting discussed the important move towards enhanced vector control strategies, such as the utilization of advanced nets, and emphasized the importance of aligning interventions with risk management and supply operations.
Context
At the 23rd Strategy Committee (SC) meeting, the scope of malaria challenges and planned mitigations were discussed as the malaria risk appetite moves to ‘high’. The Secretariat wanted to raise the SC’s awareness of the current approaches and remaining needs, in particular to advocate for support for efforts to address funding gaps and continued focus in key areas.
Against the backdrop of the global malaria response, presented during an Informal Board call on 29 September, the SC discussion focused on the Global Fund’s areas of influence. The SC discussed the current progress on malaria control and the challenges it faces, how these challenges are being mitigated and if these mitigation opportunities are enough to get the global malaria response back on track.
Malaria control: current progress
We are far from meeting the Global Malaria Technical Strategy targets, as Figure 1 shows.
Figure 1. Gaps in targeted reductions in malaria cases and deaths according to Malaria Technical Strategy targets
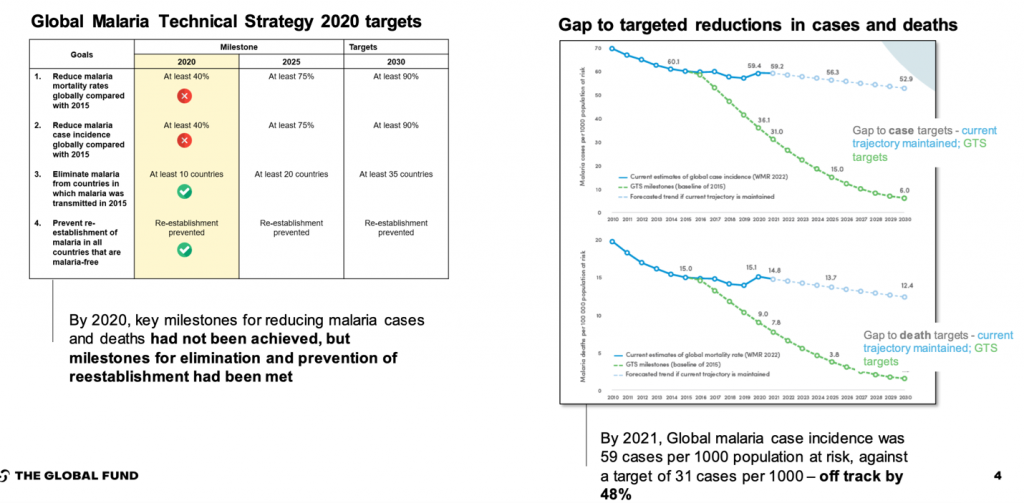
The status in Sub-Saharan Africa has plateaued. In the 11 highest burden countries, while small overall declines in absolute number of deaths there have been increase in absolute number of malaria cases (from 165 million in 2020 to 166 million in 2021).
Figure 2. Trends in SSA and highest burden countries
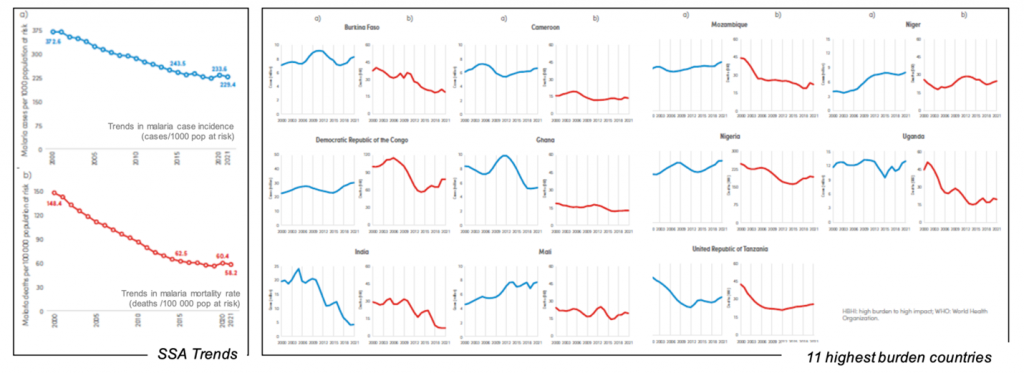
The global picture shows mixed progress.
Figure 3. Global progress in malaria control
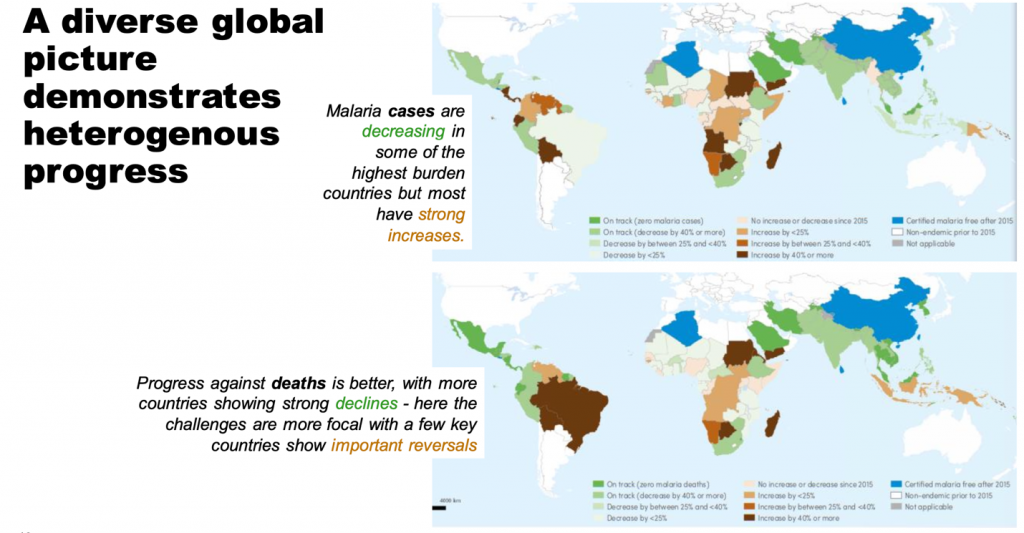
Source: Global Fund
Challenges
Low coverage of existing malaria tools, population dynamics and security issues, climate change, financial issues and biological challenges such as drug and insecticide resistance and invasive vectors are just some of the constraints. There is a complex interplay of financing and programmatic challenges:
|
Quality of programming is improving – more cost-effective but higher absolute cost |
Achieving sustainable coverage – particularly the last mile – has challenges |
Co-dependence of RSSH and malaria brings opportunities and challenges |
Financial gaps faced by all malaria partners |
|
|
|
|
These challenges were reflected in Grant Cycle 7 (GC7) funding requests (FRs)
The initial picture is already changing: all countries applying to the GF GC7 this year saw gaps in essential malaria services, mostly in Year 3. And key funding challenges persist. Malaria interventions remain underfunded especially in high burden malaria countries – this ‘struggle to tread water’ means there is an inability to innovate around delivery models of effective tools or expanded deployment of innovative malaria tools. Some examples of ITN gaps are Guinea at $17 million, the DRC at a shocking $200 million and Senegal at $20 million. Meanwhile, partners are struggling to maintain the needed geographic coverage, with some withdrawing their ITN campaign support (e.g. in DRC, Guinea, and Senegal).
Funding challenges, country-led prioritization decisions and bio-threats have combined, leading to insufficient program scope. The estimated malaria funding gap for Windows 1 and 2 is approximate $1 billion to sustain essential services (public sector case management, ITNs in high and moderate burden countries, and SMC) without factoring in the implementation of sub-national tailoring as per country national strategic plan or looking at the full optimal product selection (increasing the gap to $1.5 billion).
Actions to mitigate the challenges
Address financing challenges with partners under the leadership of malaria endemic countries
|
Explore all funding |
✓ Work with countries and partners on advocacy plans and work globally in resource mobilization. ✓ Explore innovative financing mechanisms under the leadership of malaria endemic countries. ✓ Prioritize conversations with the private sector and explore joint areas of concern e.g. climate change. ✓Explore COVID-19 Response Mechanism (C19RM) reprogramming opportunities where relevant. |
|
Optimizing investments |
✓ Sub-national tailoring of malaria interventions as per the country national malaria strategies to supporting both optimization and prioritization decisions ✓ Examine potential for efficiencies during grant making by changing product specifications, delivery models or scope of ‘supportive’ activities (such as support supervision) – but risk/benefit critical to assess. ✓Alternative financing approaches can bring efficiencies and will be further explored. |
|
Address unit costs |
✓Working with partners under the NextGen MarketShaping SI has seen a successful start with the Revolving Fund lowering CFP nets prices; there is potential for a co-financing model for specific artemisinin-based combination therapies (ACTs). ✓Move towards standardization in ITNs – important value for money opportunities, but implementation/change management challenges. |
|
Prioritize highest impact investments |
✓WHO GMP prioritization document across interventions. ✓Work with national programs, WHO and other partners to consider relative cost effectiveness and prioritize highest impact interventions as per Malaria strategic plans, includes consideration of omitting lower risk geographies/populations at greater scales than previously |
Address case management challenges
|
Diversify ACT portfolios |
✓With partners, support countries to consider Multiple First Line (MFT) strategies to delay emergence and spread of resistance. ✓ W1/W2: positive examples of countries including MFT plans, especially in countries reporting partial resistance – but insufficient in scope, particularly in countries where there is an opportunity to avoid emergence, due to large part to funding decision trade-offs, as well as needs for TA and operational support. |
|
Support surveillance for informed decision-making |
✓Support and align across partners, Therapeutic Efficacy Surveys (TES) and HRP2/3 gene deletion surveys and strong data sharing, to inform appropriate introduction of health products. ✓TES and HRP2/3 gene deletion studies budgeted and prioritized. |
|
Address critical barriers through market shaping |
✓Market barriers to scale-up AS-PY and DP, AS-AQ being considered to reduce pressure on AL*. ✓With partners, ensuring country readiness in terms of resistance mitigation strategies and framework for introduction of diversified ACTs. |
*AS-PY = artesunate-pyronaridine, DP = dihydroartemisinin-piperaquine, AL = artemether lumefantrine
Address vector control challenges
|
Scale up coverage of effective vector control |
✓Scale up to better nets has been accelerating since GC6 but the opportunity for impact from greater shift is not yet being fully embraced – (acceleration may increase through grant-making). ✓ Sub-national tailoring of malaria vector control as per the country national malaria strategies to supporting both optimization and prioritization targeting the most in need. ✓Support national decision-making around balancing coverage and tool choice. ✓Aspiration for better nets is high, challenges are around financial gaps. ✓Innovations in downstream efforts to more successful and efficiently reach coverage and usage targets, including in last mile: digitization, value stream mapping, activity-based contracting, alternative deployment modalities. |
|
Address critical market barriers to most effective tools |
✓With partners, under NextGen Market Shaping SI, lower pricing has been achieved for CFP Dual AI nets using the Revolving Facility and an innovative operating model with a smaller number of standard net specifications. ✓This has enabled an increase in expected volumes of these most effective nets, and will require ongoing discussions with countries to transition to the standard net specifications. ✓Need for more nuanced decision-making for countries around value for money. |
|
Support surveillance to enable informed decision-making |
✓Recommend maintaining entomological surveillance to support decision-making and performance monitoring. |
The malaria vaccine could be a potential game-changer
The advent of the Gavi-approved malaria vaccine, with a funding envelope of $155.7 million for 2022-2025, marks a new frontier in malaria control. However, supply constraints, high costs, and limited vaccine protective efficacy emphasize that while the vaccine is a monumental step forward, it is not a panacea. Successful implementation and maximum impact will necessitate a nuanced and integrated approach, ensuring it complements, rather than siloes, other malaria control interventions.
Will funding gaps be resolved?
Strong high-level support is critical to ensure maximal impact from available funds, advocacy for additional monies, and openness to alternative financing approaches: but these gaps will hinder malaria control progress
|
Short term |
Longer term |
|
|
Will case management challenges be resolved?
Wider partnership is responding but limited funding exacerbates the challenge; it will take time but progress will come.
|
Short term |
Longer term |
|
|
Will vector control challenges be resolved?
Good progress is being made, but further acceleration is needed; reaching longer term goals requires prioritized support to innovation.
|
Short term |
Longer term |
|
|
Stakeholder feedback
Stakeholder feedback on the malaria update underscores the lack of malaria response impact with the malaria burden plateauing and increasing in the highest-burden countries, the gravity of malaria challenges, and the urgency for cohesive action. The malaria community expressed concerns about the trade-offs in grant-making and the potential compromise in the country-led prioritization of malaria interventions due to insufficient funding and misalignment among malaria partners. They emphasized the importance of prioritization of malaria interventions according to national malaria strategic plans and robust health and community systems for effective delivery of malaria tools. They called for innovation, dedicated funding, and sustained focus on getting back on track with the GTS goals.
African stakeholders stressed the significance of local ownership in developing GF FR and country leadership in identifying its needs and priorities per malaria strategic plans, the critical role of health system strengthening, and community engagement in effectively delivering malaria tools. They commended the introduction of innovative tools such as new gen nets and malaria vaccines. They called for a more significant proportion of local manufacturing to address malaria challenges related to malaria drug and insecticide resistance. Concerns were also raised about the behavior-driven gap in the coverage of malaria interventions in certain regions, prompting a need to reassess the type of malaria tools and intervention delivery strategies.
Others highlighted the importance of ensuring that testing and treatment are accessible at the community level and in the private sector, particularly for vulnerable groups. They advocated for efficient product implementation, especially in areas with funding gaps, and underscored the importance of continued surveillance and responsiveness to drug and insecticide resistance.
Malaria technical experts welcome the push and focus of WHO’s global malaria programme in operationalizing sub-national tailoring to guide malaria-endemic countries in prioritizing tailored malaria interventions targeting the most in-need populations and highest malaria burden areas.
Several people mentioned the pivotal role of combined efforts of malaria-endemic countries, partners, and all stakeholders in addressing the vast annual funding gap for malaria. They emphasized the interconnectedness of malaria control with broader challenges such as climate change, disaster events, and instability. They called for holistic, multi-sectoral approaches, intensified advocacy, and prioritization of malaria interventions for the highest-burden areas as per country malaria strategic plans.
In conclusion
With the growing challenges, an aligned global malaria partnership approach is more critical than ever to advocate, innovate, and mitigate to support revived progress against malaria. The recent Strategy Committee Meeting discussed practical strategies and next steps; there’s a need to consult all Malaria community stakeholders both at country, regional ang Global level. The key to progress lies in blending global inclusive cooperation, strategic planning, innovative mechanisms, revamping the malaria community, including all communities and stakeholders, and evidence-based local action led by malaria-endemic countries. By knitting together innovative solutions and continued advocacy with a thorough and approachable strategy, the global malaria community can sustainably and effectively support malaria-endemic countries and advance towards a malaria-free world.
