
Enhancing Global Health Governance: The Role of Public Financial Management Accelerator
Author:
Samuel Muniu
Article Type:Article Number: 5
At the 51st Global Fund Board meeting in Geneva, Switzerland, held on April 23-24, 2024, the Global Fund Secretariat unveiled a crucial strategy for adopting Public Financial Management (PFM). Stressing the connection between co-financing and PFM, the Secretariat highlighted initiatives such as the Financial Transformation agenda and Co-link Strategy to modernize financial practices and strengthen accountability. Looking ahead, the organization plans to prioritize stakeholder education on PFM, align with the "One Plan, One Budget, One Report" vision, and integrate Supreme Audit Institutions to enhance financial oversight.
During the 51st Global Fund Board meeting in Geneva, Switzerland, on 23 – 24 April 2024, the Global Fund Secretariat shared a critical Public Financial Management (PFM) adoption strategy. This strategy offers a tailored and progressive approach to individual country contexts, aiming for sustainable and effective health interventions. Emphasizing the link between co-financing and PFM, the Secretariat highlighted initiatives like the Financial Transformation agenda and Co-link Strategy to modernize financial practices and enhance accountability. Future strategies include stakeholder education on PFM, aligning with the “One Plan, One Budget, One Report” vision, and integrating Supreme Audit Institutions (SAIs) for improved financial oversight.
The Crucial Role of Public Financial Management
A PFM lies at the heart of government systems, serving as the framework for managing resources under the oversight of the Ministry of Finance. In the context of Global Fund’s grant funding cycles, PFM plays a critical role in ensuring transparency, accountability, and efficiency in the allocation and utilization of financial resources (Figure 1).
Figure 1: Public Financial Management systems
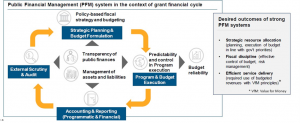
Source: Global Fund Board document GF/B51/04B
In global health financing, co-financing and PFM are interconnected elements. As countries aim to fulfill their health financing obligations and optimize investments, the alignment between co-financing and PFM becomes increasingly apparent.
Budget Formulation
At the start of the financial cycle, budget formulation guides resource allocation. Strong PFM practices, supported by transparent budget codes and robust financial management systems, ensure funds are allocated based on priorities and needs. This includes subnational planning to target investments where they are most needed.
Budget Execution
Efficient budget execution translates financial plans into outcomes. PFM systems with reliable purchasing mechanisms enable governments to track services and commodities according to priorities. Effective budget execution ensures accurate recording of co-financing, contributing to sustainability and risk management. It also facilitates country-owned verification and audit processes.
Budget Monitoring and Validation
Monitoring expenditures internally and externally completes the co-financing and PFM framework. Strong PFM systems enable effective tracking of health resources, including co-financing commitments, ensuring compliance with funding requirements. By aligning budget monitoring with impact assessment, countries can reinforce national ownership and drive efficiency in health spending. Robust monitoring and audit systems mitigate risks and support donor alignment, enhancing visibility of health resources for effective planning.
Strong PFM systems bring several benefits for governance and financial management. They focus on strategically allocating resources according to government priorities and maintaining fiscal discipline by controlling budgets and managing risks effectively. Moreover, they ensure efficient service delivery by using budgeted revenues wisely based on Value for Money principles.
Government implementers received a significant allocation in Global Fund’s Grant Cycle 6
During Grant Cycle 6 (GC6), the Global Fund allocated $18.211 billion across 122 countries, utilizing a combination of governmental and non-governmental entities for implementation. The Government Principal Recipients (PRs) were responsible for executing programs in 82 countries, comprising 67% of all participating nations. These Government PRs received a significant share of the budget, amounting to $10.601 billion, representing 58% of the total budget (Figure 2). In the remaining 33% of countries, the Global Fund engaged non-governmental PRs. The fact that the Government PRs are getting the lion’s share does not preclude some of them also taking control of the NGO PR funding, as this Aidspan article shows.
Figure 2: Global Fund implementing entities
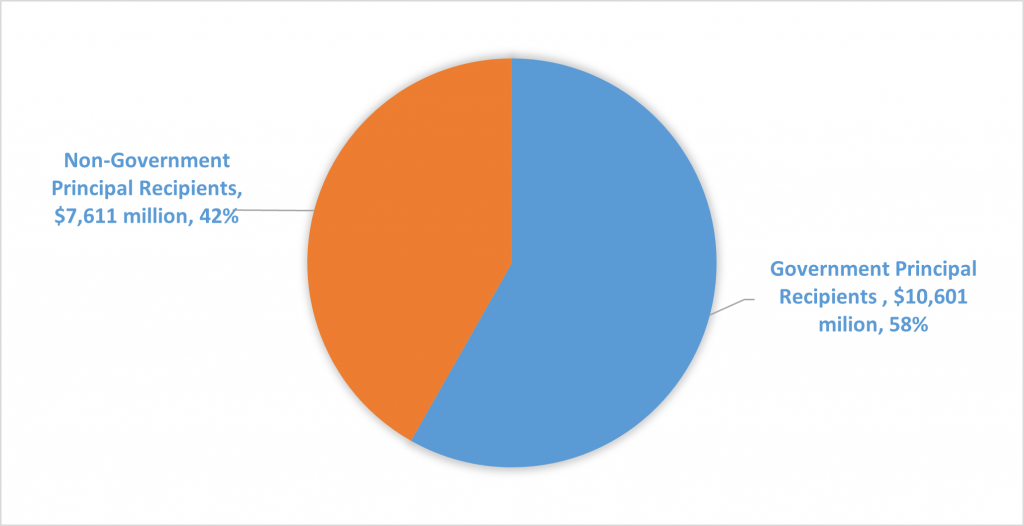
Co-link lays the foundation for catalyzing financial transformation for enhanced Public Financial Management
Between 2012 and 2014, the Global Fund initiated its Financial Transformation agenda to modernize financial management practices. This initiative, driven by the recognition of the need for systemic change, facilitated further progress in PFM. It accomplished this by actively assisting countries in developing their financial management capacity to enhance efficiency, accountability, and transparency in monitoring and reporting health spending.
In 2015 and 2016, an analysis of Financial Management System (FMS) issues led to the development of the Co-link Strategy, which focused on routine financial management, donor harmonization, and public financial management. In 2017, the Secretariat officially launched the “Strengthening Country Link Project,” or the Co-link initiative, seamlessly integrating it into the Resilient and Sustainable Systems for Health (RSSH) strategy. This project emphasized three key pillars: PFM, donor harmonized systems, and routine financial management, with a strong emphasis on capability building. By aligning diverse stakeholders and resources, Co-link actively laid the groundwork for accelerated progress in PFM adoption.
The Secretariat implemented the first phase of the project from 2017 to 2022, yielding significant results. Notable achievements included a 22% increase in budget absorption, successful resource alignment for HIV in 52 countries, and the deployment of systems in 17 Francophone nations. Additionally, SAIs conducted 16 audits of Global Fund grants, while 14 mobile money pilots were implemented. Furthermore, donor-harmonized and PFM systems for Global Fund grants were piloted in eight countries, covering all the targeted nations.
In 2022 and 2023, the PFM Maturity Assessment meticulously mapped PFM components and conducted an in-depth assessment of people, processes, and systems, laying the groundwork for capacity development and targeted interventions. Looking ahead to today, Co-link remains a linchpin in the comprehensive PFM Engagement Strategy, characterized by its scalability and contextual relevance. This strategy actively brings together stakeholders from Community-Based Organizations (CBOs), Civil Society Organizations (CSOs), government representatives, Ministries of Finance, SAIs, and more, fostering collaboration and inclusivity, thereby paving the way for sustainable PFM strengthening efforts.
Strengthening Public Financial Management: A Key Component of the “One Plan, One Budget, One Report” Vision
In global health governance, policymakers are increasingly focusing on a unified approach. They aim to streamline planning, budgeting, and reporting under the “One Plan, One Budget, One Report” (3 ONEs) vision. PFM serves as a linchpin in this process, enabling the implementation of each component.
One Plan
Effective PFM systems support the development of unified, country-wide strategic plans for the health sector. By facilitating stakeholder engagement and ensuring transparency in resource allocation, PFM enables the creation of comprehensive and coordinated health strategies.
One Budget
PFM systems consolidate resources from various sources, including public funding, donor contributions, and NGO support, into a singular budget aligned with strategic health objectives. Through efficient budgeting and financial management, PFM ensures that resources are allocated judiciously and in line with the priorities outlined in the strategic plan.
One Report
PFM systems enhance governance, oversight, and accountability in fund management, leading to improved tracking of co-financing commitments and domestic resource allocation to health. By standardizing reporting processes and enhancing transparency, PFM enables better legislative oversight and ensures that public funds are disbursed and utilized responsibly.
While ideal PFM standards are clear, they vary in different countries. The Global Fund must find a balance between the ideal and what’s practical, considering each country’s unique challenges. To bridge the gap between theory and practice, the Global Fund plans to educate stakeholders on PFM through workshops. These workshops will involve country leaders, Budget Directors, and partners, aiming to create a shared understanding of PFM and its relevance to different contexts. Collaboration and flexibility are essential as the Global Fund works towards enhanced PFM and the 3 ONEs vision. By leveraging stakeholders’ expertise, the Fund can navigate global health governance complexities and drive progress towards better health systems. Through strategic investments in PFM and efforts to promote alignment with other Global Health Initiatives (GHIs), the Global Fund can improve health outcomes for all.
A Roadmap for Effective Public Financial Management Implementation
Achieving robust PFM systems requires a strategic and tailored approach that considers the unique context and challenges faced by each country. In the short term (3 years), there’s an assessment and capacity-building phase (Figure 3). This is followed by a focus on donor harmonization (3-5 years) to align efforts with major donors. Medium to long term efforts (5-10 years) prioritize strengthening public financial management systems, and finally, in the long term (10+ years), the aim is sustained adoption of effective financial management practices integrated into governance structures.
Figure 3: A journey to effective PFM implementation
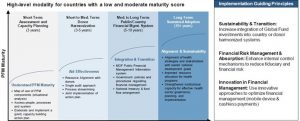
Source: Global Fund Board document GF/B51/04B
Implementing PFM successfully relies on key factors. It’s important to align health strategies with stakeholders to ensure sustainability. Assessing PFM maturity and making a capacity-building plan are crucial for progress. To enhance aid effectiveness, synchronize resources with donor priorities and streamline processes. PFM should closely adhere to national development goals to improve resource allocation and institutional capacity.
Understanding PFM Maturity in Global Fund Portfolios
PFM maturity is a measure of the level of advancement in a country’s financial systems. As countries navigate the complexities of health financing, it becomes essential to gauge their PFM maturity to inform strategic interventions and drive progress. Global Fund PFM maturity baseline reveals a diverse adoption journey, spanning from the short-term to the long-term, with varying levels of maturity across different portfolios (Figure 4).
Figure 4: PFM Maturity in Global Fund Portfolios
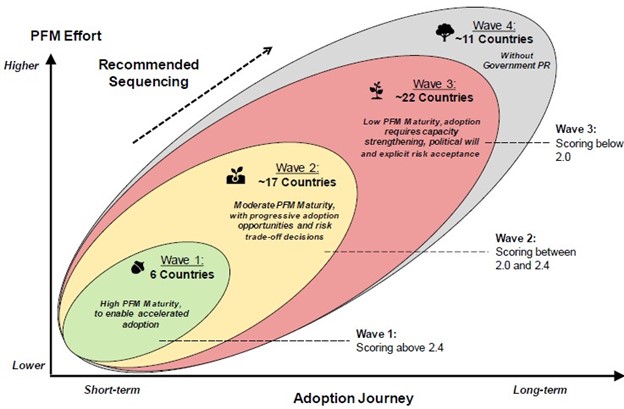
Source: Global Fund Board document GF/B51/04B
PFM maturity is vital for implementing the “3 ONEs” framework across diverse country contexts. Rwanda and Ethiopia serve as examples, each striving to improve their health sector planning and budgeting processes. Rwanda follows a structured approach, starting with priority setting and strategic planning using the Medium-Term Expenditure Framework (MTEF), and ensures transparency through performance-based funding from the Global Fund. Rwanda’s integrated financial management system and internal oversight mechanisms bolster transparency and accountability. In contrast, Ethiopia adopts the “3 ONEs ” principles under its Health Sector Transformation Plan (HSTP-II), consolidating activities into a unified plan to enhance coordination. Stakeholders align their inputs with the broader sector plan, and the Global Fund funding is managed through the national PFM system, ensuring alignment with the health sector strategic plan. Both countries aim to enhance efficiency and transparency, albeit through different approaches.
Understanding the interplay between PFM maturity and the implementation of the “3 ONEs” is crucial for achieving desired outcomes. Out of 17 countries studied, around 40% have a good level of PFM maturity. This means they’re in a good position to use their financial management skills to help achieve the 3 ONEs. However, it’s important to adapt the methods used to ensure everything fits the specific situation of each country. Currently, about US$3 million is given directly to non-governmental groups. Understanding how these groups are impacted by the 3 ONEs and how effective the government’s methods are in hiring them is crucial. For the 40% of countries with low PFM maturity, further analysis is needed to figure out the best ways to provide support and coordinate efforts among different groups.
Integrating Supreme Audit Institutions into the PFM Roadmap
PFM is crucial for effective governance, ensuring transparency, accountability, and efficiency in handling public resources. SAIs are key players in this framework, providing independent assessments of government financial practices. Integrating SAIs into the PFM roadmap is vital for bolstering assurance and accountability (Figure 5).
Figure 5: Four pillars of the Global Fund’s Supreme Audit Institution Engagement Strategy

Source: Global Fund Board document GF/B51/04B.
The SAIs, as mandated by constitutions of their respective countries, audit government finances, offering assurance to stakeholders and identifying areas for improvement. Active engagement involves collaboration among government, development partners, and SAIs, aligning audit priorities with PFM goals. Strengthening SAIs through capacity-building and legal support enhances their effectiveness and independence. This integration enhances assurance and accountability by detecting fraud, waste, and inefficiencies, ultimately improving governance and service delivery.
Stakeholders feedback
Through written statements, some stakeholders endorsed the Global Fund’s efforts to improve PFM. They believe that by enhancing transparency in co-financing and providing capacity building for SAIs, the Global Fund can contribute to sustainable domestic financing. This viewpoint suggests confidence in the effectiveness of the Global Fund’s strategies and underscores the importance of efficient PFM in achieving financial sustainability.
However, other constituencies expressed concerns about the adaptability of the PFM framework, particularly within the context of the 3 ONEs approach. They highlighted significant differences among countries regarding budget definitions, procedures, responsible agencies, and financial reporting. This apprehension indicates a need for greater flexibility and customization to address the diverse contexts and challenges faced by individual countries.
Secretariat feedback on PFM and sustainability
The Secretariat clarified that they don’t lead the PFM reform; instead, it’s mainly driven by institutions like the World Bank and the International Monetary Fund (IMF). Their focus is on making sure grants are integrated well into national budgets to improve fund management. They stress using funds effectively within countries to avoid unspent money going back to the national treasury. Collaborating closely with global health partners like the World Health Organization, they ensure that PFM and sustainability strategies consider the broader health ecosystem and meet global standards.
Efforts are underway to gradually integrate the ‘One Plan’ into programs, with workshops to help with understanding and implementation. The Secretariat sees PFM as a tool for sustainability, aiming to help countries keep up health outcomes even without external funding. They highlighted the importance of finance ministers understanding how funding changes affect health and education.
In response to queries about aligning with agencies like the World Bank, the Secretariat acknowledges differences but focuses on a tailored strategy based on disease burden and country needs. They promise quick support for countries rather than long policy discussions, emphasizing the urgency of keeping up health impacts. Finally, they stressed the need to adjust strategies to handle changing circumstances effectively and address sustainability challenges.
Board Document GF/B51/04B, Strategic alignment: Public Financial Management Accelerator, should be available shortly at https://www.theglobalfund.org/en/board/meetings/51.
